The PATH forward: How pharma can drive four key healthcare trends
The field of healthcare is transitioning from an old traditional model to a future model characterized by innovation. Healthcare is undergoing a transformation like never before. Driven primarily by advances in data and digital technology, the way healthcare is developed, sold, used and discussed, is fundamentally changing.

Of course, healthcare is extremely complex and multifaceted, and this is further exacerbated by differences in national and regional approaches, infrastructure, funding etc. But there are some broad trends and commonalities that cross geographies and therapy areas, many of which pharma is in a unique position to help drive forward.
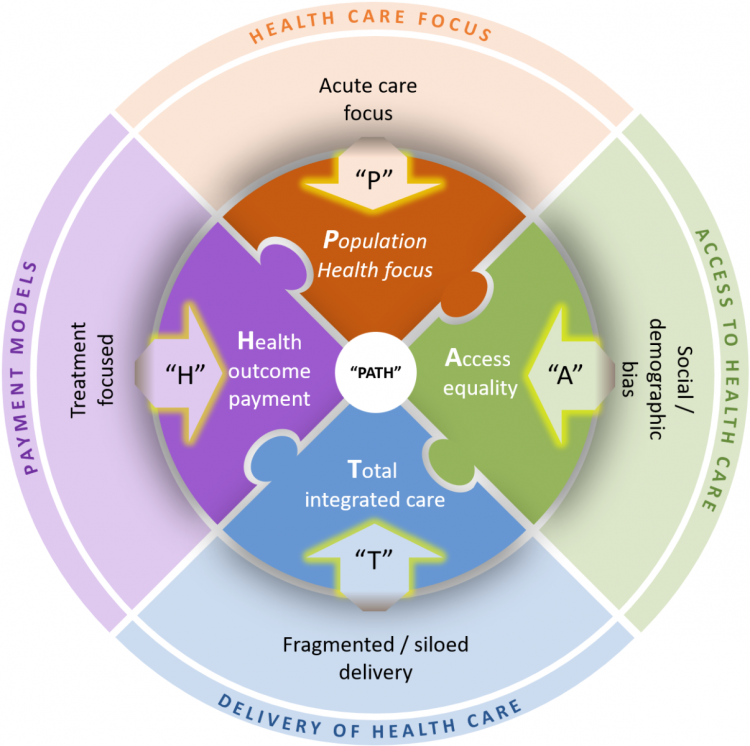
This article focuses on four specific trends – using the acronym PATH – where the field of healthcare is transitioning from an old traditional model to a future model characterized by innovation:
- Population health focus
- Access equality
- Total integrated care
- Health outcome payments
Below we examine these one by one and see how pharma companies can not only navigate through this PATH but thrive by leading the way.
Population health focus
The population health approach describes a shift in healthcare systems from a narrow model of acute care for individual patients, to one that focuses on the health and overall wellness of the broader population (Cohen, 2014). It represents a shift away from reactive to proactive healthcare, promoting healthcare of communities at large.
It is necessary because with ageing populations and improvements in acute care, non-communicable diseases (NCDs) have become more prevalent and harmful to society. Indeed, the World Health Organization (WHO) estimates that NCDs kill 41 million people each year, equivalent to 71% of all deaths globally. And they impact all ages – each year, more than 15 million people die from a NCD between the ages of 30 and 69 years, with 85% of these "premature" deaths occurring in low- and middle-income countries.
The current model is not set up to proactively manage NCDs, which means an expensive reactive approach, which is worse for patients, healthcare systems and society. In the US alone, the total cost associated with chronic diseases is estimated at $3.7tn, close to one-fifth of the entire US economy.
New approaches are needed. In England for example, population health has been described as the ‘driving force’ behind new Integrated Care Systems. Now, pharma companies need to adapt their offer accordingly. A fundamental shift is required from being the ‘provider of pills’ to a ‘genuine partner for population health’.
Some are already taking this path. In 2021, an agreement between Novartis and the NHS in England aimed to enable broad and rapid access to cholesterol-lowering medicine Leqvio® (inclisiran) via a population health management approach identifying eligible patients across the country. The Novartis population health management approach is anchored in building partnerships between Novartis and systems of care around the world that accelerate patient access to a therapy, with the goal of improving the cardiovascular health of the system’s defined population at speed and scale.
Pharma companies need to plan early to ensure pivotal clinical trials and wider offerings beyond the pill reflect the unmet needs throughout the patient journey, and particularly in preventative and early-stage care, companies must be able to show that innovative treatment approaches will save funds further down the line.
Access equality
The significant health inequalities that exist all over the world have been well-documented. On a macro scale, the biggest inequality exists between high and low-income countries.
People born in high human development (HD) countries have 19 years higher life expectancy than people in low HD countries.
But there are a host of other non-medical social determinants of health (SDH) that influence health outcomes – the conditions in which people are born, grow, work, live, and age, alongside the wider set of forces and systems shaping the conditions of daily life all come into play.
The COVID-19 pandemic starkly exposed how existing inequalities are associated with an increased risk of becoming ill with a disease such as COVID-19. For example, racial and ethnic minority groups were disproportionately affected both in the US and in Europe by the pandemic.
Now that health systems are starting to acknowledge that addressing SDH is key to driving meaningful health improvement across populations, there is a significant opportunity for pharma to play an important role. Initiatives aimed at ameliorating social risk factors, from clinical trial design through approval and beyond will be greatly differentiating and further serve the drive towards population health and improved outcomes.
SDH can be incorporated into clinical trial designs and real-world evidence creation, improving trial data transferability into clinical practice across wider populations and to support policymakers in their decision-making process. Companies can also implement solutions beyond trials, such as analyzing data obtained on SDH to drive preventive and predictive strategies or developing resources to support healthcare providers, patients and caregivers in advancing health literacy.
Pharma "PATH" forward: 4x key health care trends
Total integrated care
Broadly speaking, integrated care is a principle where the needs of the patient or population are central, and the healthcare services and solutions work in a coordinated and flexible way around it. To achieve greater population health and health equity, the need for enhanced integration in healthcare is more significant than ever.
Interconnectivity of healthcare professionals (HCPs) can play a big role in increasing quality of care and reducing medical care costs. One US study in the cardiovascular disease space for example, showed that primary care teams who made treatment decisions as part of an integrated network, resulted in a reduction of cardiovascular disease-associated hospital days by 38% and a reduction in average spend per patient over 12 months by $516.
For pharma companies, integrated care means interacting with a complex ecosystem of stakeholders, not just individual HCPs in silos. The biggest shift underway within pharma companies is one of mindset. The role of pharma is moving away from simply bringing products to market, towards providing holistic solutions for better patient outcomes. This requires identifying the required outcome first and working backwards from there.
Fresenius Medical Care – the world’s leading provider of products and services for people with chronic kidney failure – is an example of a company thinking in a more holistic way. The company aims to closely mesh treatments and solutions over the entire path of the illness. Its strategy encompasses three key areas – the Renal Care Continuum of dialysis products and services, critical care solutions, and complementary assets.
Pharma can support the evolution of healthcare from a fragmented to a more integrated system by initiating local pilots of dedicated disease specific care networks, which may be centered around dedicated case managers. These case managers could help to select patients for which case management is most appropriate, ensuring regular monitoring and adjustment of care as necessary, with the pilot results making the case for subsequent broader roll-out.
Health outcome payments
With healthcare budgets under greater pressure than ever, healthcare systems around the world are seeking to achieve the best possible value from their investment. But value is notoriously hard to define, measure and demonstrate.
With ever-more complex care-pathways and more diverse stakeholders involved in care, the elements driving a clinical outcome become even more difficult to untangle. And the number of potential factors that could undermine that outcome – whether that is lack of integrated care, misalignment between patient and provider, patient adherence, or something else – increase further.
In a golden age of pharmaceutical innovation – which includes high-priced single-use cures – it is in pharma’s interest to link payment to value. The industry just needs to get better at measuring and demonstrating this value in a real-world, population health setting.
Stakeholders in healthcare are increasingly turning to real world evidence (RWE) to inform their decisions, alongside evidence from randomized controlled trials (RCTs). To help inform the value of RWE, pharma companies need to develop standards and processes for each stage of the evidence generation pathway. RWE needs to become a core element of company corporate strategy, ensuring a long view and maximum quality of data and evidence.
With more robust RWE to demonstrate value, pharma companies can further embrace innovative payment models that have value at their core.
Conclusion
As the field of healthcare continues to evolve at a rapid pace, pharma companies need to focus on the elements they can influence and shape. The four areas presented in this article are all interlinked, representing a more holistic and collaborative approach for pharma companies, moving away from a provider of pills towards a genuine partner to health systems around the world. It is on this PATH that companies can provide and generate the most value and improve care.
Original article published in PME magazine:
https://www.pmlive.com/pme#/reader/45430/153528