Digital healthcare may revolutionise management of chronic diseases, but who is going to pay for it?
With approximately half of all adults worldwide living with a chronic condition, providers are looking at digital solutions to transform this area of healthcare

Digital healthcare is a booming industry. According to one recent report, the global digital healthcare market is projected to grow from an estimated $147 billion in 2019 to $234.5 billion in 2023. If we look at apps alone (which is just one element of digital healthcare), there are now more than 300,000 health-related apps available – more than double the amount five years ago.
Much of this growth is being driven by the urgent need to innovate in chronic diseases such as cancer, diabetes, mental illness, heart disease, and respiratory disease. Approximately half of all adults worldwide today are living with a chronic condition, and global spending on chronic conditions is projected to reach a healthcare-system bankrupting $47 trillion by 2030.
The extraordinary costs are largely driven by the complexity of managing chronic conditions – the multiple healthcare personnel involved, the burden of regular review and follow-up, the difficulties around patient self-care and management, the administrative burden – and it is hoped that digital healthcare solutions will prove transformative in this area.
But while the rationale and transformative potential of digital healthcare solutions are undeniable, who’s going to pay for them, how and under which circumstances?
Digital healthcare - a very broad umbrella
But first, let’s just take a step back a moment. What exactly do we mean by “digital healthcare”?
It’s a term that encompasses a very wide range of areas and solutions. The World Health Organization (WHO) defines digital health as “a broad umbrella term encompassing eHealth (which includes mobile health), as well as emerging areas, such as the use of advanced computing sciences in big data, genomics and artificial intelligence”.
Such definitions offer multiple ways to categorise digital health solutions depending on the objective and criteria. These categorisations can include where they are used along the patient journey (e.g. prevention and screening, diagnosis, treatment, disease management), the type of technology used (e.g. 5G, AI, blockchain, diagnostics & omics), the type of application (e.g. disease knowledge, remote monitoring, telehealth, predictive analytics) .
The Digital Therapeutic Alliance has proposed a categorisation based on level of risk and corresponding levels of necessary evidence and regulatory oversight:
- Digital health (e.g. user-facing technologies such as lifestyle apps and fitness trackers, which require no regulatory oversight)
- Digital medicine (e.g. digital diagnostics and biomarkers, where requirements for regulatory oversight vary)
- Digital therapeutics (e.g. interventions to prevent, manage or treat a condition, which must be reviewed and certified by regulatory bodies)
This categorisation may be a useful one as it puts the onus on evidence and outcomes, which helps to define value. This is an essential step in overcoming funding barriers for digital health.
Who’s paying for what?
According to the WHO, funding is the main barrier to implementation for most of the digital innovation solution categories.
It is useful to assess digital health solutions by two key parameters: their scope of application (e.g. do they apply to the whole population or one single patient?) and the setting in which they are used (e.g. are they used in the outpatient setting by the patients themselves or by/with healthcare professionals (HCPs) in the hospital or clinic?).
These parameters have been used to create the grid in Figure 1, the color coding signifying the associated level of difficulty with funding.
Figure 1: Different types of solutions correspond to different reimbursement/funding pathways
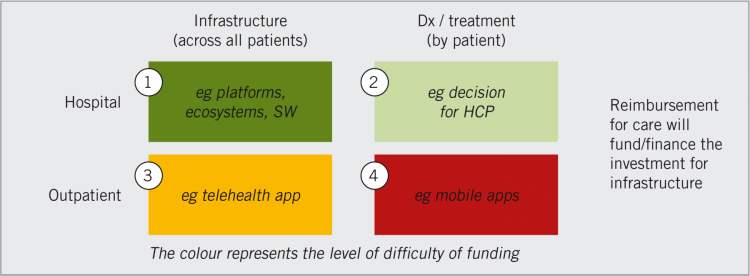
Solutions in the first quadrant – applicable to all patients and used in the hospital setting – are the most straightforward and can be funded by the hospital, clinic or practice budget, if the budget is available.
Solutions in the second quadrant can be funded through the diagnosis-related group (DRG) hospital payment system. The payer in this instance is the insurance company or national health system. These solutions are considered relatively straightforward to fund if the cost does not have a significant impact on the DRG amount (which is capped) and on the margins.
It is the third quadrant where things start to become a bit more complicated. In countries that utilize tariff systems, solutions could be funded in the context of the procedural tariffs that healthcare professionalsHCPs use for consultations. On one hand, this should be relatively simple as a consultation or activity should not depend on the channel or the technology used to deliver it. On the other, this is actually the biggest barrier in some countries because codes for telehealth and telemedicine have not been introduced and therefore healthcare professionals are not remunerated for a virtual visit. For some products used in the context of the consultation, one will also need to establish what goes to the physicians and what to the manufacturer.
Solutions in the fourth quadrant would need to be funded as stand-alone solutions as they are not medical acts and they are mostly used by the patients. The payer is the insurance company or national health system. Germany appears to be embracing this approach with its new Digital Health Applications (DiGa) Fast Track system, establishing a right for digital health solutions to be prescribed and reimbursed by insurance companies.
Payment models of the future
Several innovative mechanisms of payment and reimbursement are starting to emerge, including some being trialled in France as part of the country’s Article 51 experiment, which uses new financing and organizational methods to enable innovation.
The Article 51 pricing models include:
- Episodes of care (EDS), which aims to set up a global bundle for a surgical care episode
- Incentive for shared care (IPEP), a population-based payment, which aims to collectively encourage HCPs to organise themselves by setting up groups to implement actions on behalf of populations
- Payment in team of HCPs (PEPS), an integrated care payment that aims to test a new model of collective lump-sum financing for HCPs.
These models require systems and care to be integrated, which is also something that digital health is trying to support. But because systems are generally not yet fully integrated, and because to benefit from those mechanisms one will need to “own” the patient care or collaborate with whoever does own that responsibility, pricing for digital health solutions still relies on models that are typical of software e.g. pay per use, flat rates, subscription, freemium, license fees.
Establishing value, of course, necessitates assessment – whether that’s through a health technology assessment (HTA) style procedure or something else. Currently, very few initiatives and guidance for formally evaluating digital health are available. But it’s important to recognize the distinct differences between pharmaceuticals and digital health solutions, which not only depend on clinical and economic aspects but also on technical features, perceived benefits for healthcare managers, willingness to use by end-users, and finally, the healthcare system’s capacity to benefit from the innovation (Kolasa, 2020).
Modernizing evidence generation for digital healthcare
For assessment of digital health solutions to be successful, there is no doubt that more pragmatic ways of developing evidence are needed. Traditional methods of evidence generation – such as prospective studies and systematic reviews – are not well suited to the agile approach taken in software/tech development. In fact, the use of traditional approaches for the evaluation of digital health solutions has been identified as a major obstacle for their wider adoption (Guo, 2020).
Innovative approaches, such as simulation-based research, should be considered, including computational, system, and clinical simulation (Guo, 2020).
Germany has been one of the first countries to act. On April 21, 2020, the ‘DiGAV’ came into force, providing pragmatic approaches for providers of digital health solutions. For example, demonstrating proof of positive healthcare effects can be provided via a retrospective intra-individual comparison, showing the benefit of using the digital health application (compared to not using it). And if the provider is not yet able to prove positive healthcare effects, it can ask to be considered for evaluation on expected positive healthcare effects based on “plausible grounds” and impartial scientific evaluation.
It is this kind of pragmatic approach that will help to facilitate more widespread adoption of digital health solutions.
Conclusions
Digital health is a fast-evolving field, but its huge transformative potential means that urgent questions need to be asked. For regulators, why should the channel or technology with which we deliver care really matter for reimbursement? It’s surely the outcome that matters. If the evidence is there, why not let HCPs choose how to deliver optimal care? Tech thrives on competition – why not unleash this in the healthcare sector to drive up quality and value for money?
For the biopharmaceutical industry meanwhile, it is a case of keeping pace with the latest developments. The sheer heterogeneity of digital health solutions will inevitably lead to multiple different pathways of funding and reimbursement depending on the application and the setting of use of the solution. But there is one constant and that is the need to demonstrate value, even if the pricing models are similar to those of software and other tech. Ultimately, as is the case in France and Germany, more pragmatic ways of developing evidence and recognizing value will continue to emerge and be applied to digital health in the future. If so, there is a significant opportunity for companies to establish unique and differentiating offerings with digital health platforms for their product portfolios.
References
Guo C, Ashrafian H, Ghafur S, et al. Challenges for the evaluation of digital health solutions—A call for innovative evidence generation approaches. Digital Medicine. 2020; 3:110
Kolasa K and Kozinski G. How to Value Digital Health Interventions? A Systematic Literature Review. Int. J. Environ. Res. Public Health; 2020, 17, 2119







