Access & reimbursement to reward innovation in digital "BTP" solutions
Emerging digital technologies are one of the fastest growing sectors within the healthcare industry and are starting to reshape our perspective on how some diseases can be managed. Utilizing big data, sensors, artificial intelligence and software platforms provides the opportunity for improved disease management across multiple therapy areas. Pharmaceutical companies are aware of this opportunity and are looking at ways in which these types of technologies can complement their products to offer “beyond the pill” solutions.
Until now, many of the currently available digital technologies within the healthcare sector have targeted patients as the consumer and customer, meaning most technologies are paid by patients out-of-pocket or offered for free by manufacturers or pharmaceutical companies. This situation is not ideal for uptake or innovation and it is driven by the lack of clear MA pathways in most countries, which pose a hurdle for manufacturers trying to deliver solutions and benefits to patients. Only a few Health Technology Assessment (HTA) bodies in Europe have already started to investigate how they can evaluate digital technology solutions alone, or in combination with pharmaceutical products.
Nevertheless, there are some exceptions where digital solutions have achieved reimbursement via similar processes as used for pharmaceutical products, yet only a limited patient population have access to these. With the current analysis, the objective was to understand if and how these exceptions can become the standard and what could be a roadmap for policy makers, payers and manufacturer to achieve universal reimbursement for digital solutions in healthcare.
Current reimbursement landscape
An internal database of currently available and developing digital health technologies was created through secondary and primary market research of the current landscape. Technologies added to the databased included: digital health monitors, software platforms (applications or web based), or technologies which provided patients access to remote healthcare professionals. All of the technologies could have a single component (standalone), be combination solutions incorporating multiple technologies, be associated with pharmaceutical products, or be a medical device. For the analysis, only digital technologies which were commercially available and had evidence of access were used, including paid for out-of-pocket, provided free of charge or reimbursed.
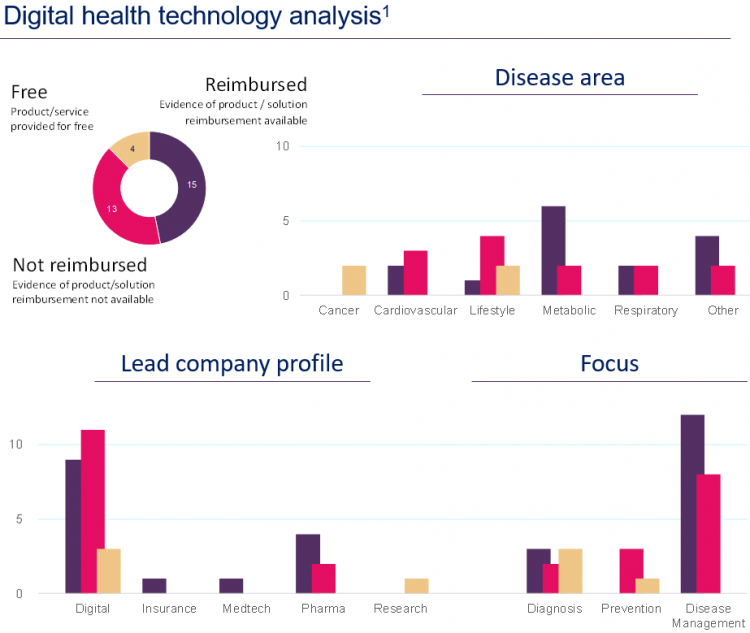
From the sample of 32 products included in the analysis it is clear that manufacturers are driven to developing a variety of innovative solutions that can optimize care through improved diagnosis, real time disease management and remote access to health professionals.
The target disease areas are usually prevalent and chronic ones, such as metabolic and cardiovascular diseases where innovative solutions can have the greatest impact.
The developers of most technologies are digital companies, however, pharmaceutical companies are also involved in many partnerships and acquisitions of digital health developers.
In terms of reimbursement, from the technologies analyzed there is evidence that around half are reimbursed or partially reimbursed in some way. However, in most cases it seems that reimbursement is highly fragmented and de-centralized due to a lack of clear reimbursement pathways. Out of the reimbursed cases, some technologies are funded through specific channels such as hospitals, insurance companies and employers.
It seems that in countries that operate with an insurance based reimbursement system (Germany, USA, Switzerland) access can occur insurance by insurance, while in national systems, such as UK and France, there is some sort of centralized process. In France the process is the same as for the medical devices while in UK an ad hoc process was established under the new Innovation & Technology Tariff. With the new system in the UK, the NHS Innovation Accelerator (NIA) regularly screens and analyses proposals by manufacturers where the Innovation & Technology payment system provides a separate funding pathway. From the countries analyzed it could be considered that the UK is advanced in terms of digital technology assessment and providing dedicated funding. This funding mechanism follows the NHS’s “zero cost” model, which provides top-up funding to existing CCG budgets, creating a separate funding pathway. 4&5
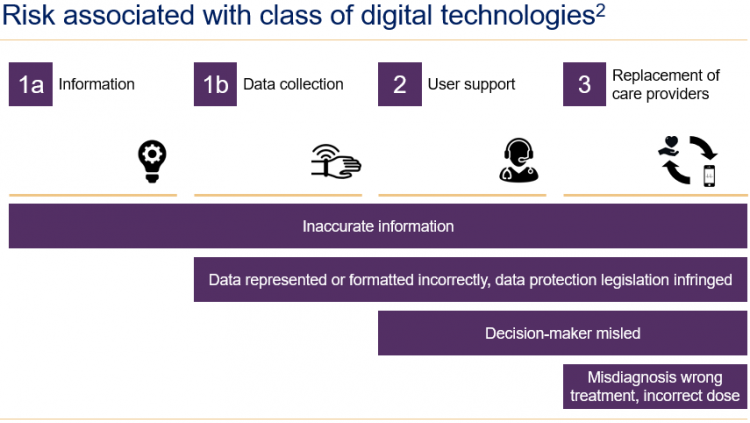
Yet, the main commercialization consideration for digital health technologies is to achieve regulatory approval as a medical device. For developers, the evidence requirements to achieve CE marking is clear even if challenging, especially for companies that have little experience. In contrast, the evidence requirements from a reimbursement perspective are unclear.
Often developers reach the market with their technologies and have insufficient data to seek reimbursement or prove their value. The current scenario can be compared to the pre-HTA environment of the pharmaceutical industry, where proving clinical benefit of a product was more important than demonstrating value for money or cost-effectiveness. Over time, the pharmaceutical industry and HTA agencies have evolved and now Market Access is a key consideration in the commercialization strategy for any manufacturer. This could be taken as a learning for the developers of digital health technologies.
Key developments and evidence requirements
Although there are currently some limitations and challenges to the reimbursement landscape of digital health technologies, this is also creating opportunities for forward thinking companies to differentiate themselves from competitors. The value that digital health technologies can bring in terms of optimization of care and cost savings is also not going unnoticed by some HTA bodies and insurance companies who are looking to reward developers of such technologies where they see value. As mentioned before, some HTA bodies are developing processes to formally assess digital technologies in a move to support access. In the UK, as of March 2017 NICE introduced an assessment process for the digital health technologies, which will provide transparency to developers in terms of data requirements for reimbursement.4&5
An example of success comes from Livongo Health, a Californian start-up, who achieved successful reimbursement with a number of insurers in the US for their $50 per month diabetes program, which now has over 35,000 users. Their diabetes program combines consumer health technology, data insights, and real-time support and Livongo is now seeking to expand into Europe. Livongo’s success can first be attributed to its early adopters who paid out-of-pocket, this contributed to creating an image that the product had value and was user friendly for patients. Moreover, Livongo had the ability to generate the necessary evidence for a broader population coverage of its diabetes program by insurances. In Livongo’s case, during clinical trials in the development phase they planned to generate payer meaningful evidence like cost savings data, reduction in hospitalizations and reduction in hypoglycemia, to allow payers to evaluate the value of their technology and make reimbursement decisions.3&6 Another relevant example is MyCOPD, an app that allows patients with Chronic Obstructive Pulmonary Disorder (COPD) to self-manage their condition on their phone or tablet, which has been reimbursed in the UK through the NIA.5
Conclusions & recommendations
Going forward it will be important for the developers of digital health technologies to integrate health-economic evidence generation and payer value communication activities into their commercialization plans. This will be important even if the reimbursement pathways in many markets need to catch-up with the innovation of these technologies. Parallels can be drawn from the access and reimbursement evidence requirements of their pharmaceutical counterparts.
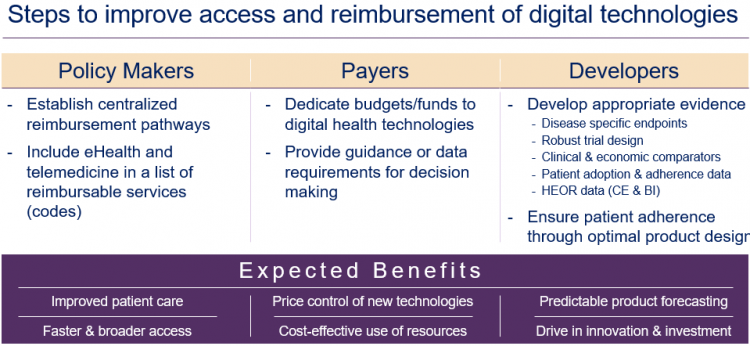

Developing structured access and reimbursement pathways for digital health solutions will likely have a number of positive effects for the healthcare industry across multiple stakeholders types. Broader access will allow more patients to benefit, HTA bodies to have control on the pricing and reimbursement of these type of solutions, whilst stimulating additional appetite for innovation and investment within the sector.
References
1. Executive Insight Digital Health Technology Database; accessed 30.10.2017
2. Guidance document Medical Devices - Scope, field of application, definition - Qualification and Classification of stand alone software - MEDDEV 21/6; European Commission; 15.07.2016
3. Digital disrupters take big pharma ‘beyond the pill’; Sarah Neville; Financial Times; 24.04.2017
4. https://www.digitalhealthdownload.com/2017/02/nice-introduce-hta-style-app-assessment-process-march-2017/; accessed 30.10.2017
5. https://www.england.nhs.uk/2016/06/treatment-innovations/; accessed 30.10.2017
6. www.livongo.com; accessed 30.10.2017









