No incentive for a cure – Part 2
A delicate balance: solutions for cost-effective but unaffordable medicine
How much is a cure worth?
In a previous article, we explored the dilemma of how to price, pay for and incentivise, ground-breaking treatments that are given once, or in the short-term, and completely cure previously incurable diseases.
The WHO states that a fair price is one that is “affordable for health systems and patients and that at the same time provides sufficient market incentive for industry to invest in innovation and the production of medicines.”
But there is a paradox at the heart of many innovative curative therapies – while they are cost-effective over the long-term, they are unaffordable in the short-term.
One could argue that it is the duty of society to ensure that healthcare systems can keep pace with science to ensure life-saving innovations are accessible to the people who desperately need them. But at the same time, healthcare budgets are finite, and we also have a duty not to bankrupt healthcare systems.
So, what do we do?
In the previous article, we talked about two broad choices; either incremental solutions, implemented in the confines of existing health systems and reimbursement environments, or sweeping systemic solutions, which reimagine systems to fit the scope of science’s ambition.
In this article, we will examine some of the incremental solutions currently being championed by various stakeholders.
Square pegs, round holes?
If fitting expensive, one-off medicines into health systems designed for chronic diseases is a bit like trying to put square pegs into round holes, then incremental solutions are like chiselling away at the peg, the hole, or both, to force them to fit. It won’t be a smooth fit, but it might just about work.
So, which incremental solutions have been attempted, and which are working well? We have selected four examples – each one championed or led by a different stakeholder.
Policy makers: Staged access and delisting
Sovaldi (sofosbuvir), a cure for Hepatitis C (HCV), is a well-known example of the “cost-effective but unaffordable” paradox. It is associated with extremely impressive cure rates – as high as 97% in combination with ravidasvir – and the money saved in the long-term makes it good value, but its initial $1,000-a-pill pricing caused significant backlash.
On its launch, high demand led to a surge in demand, causing significant anxiety among payers. Gilead’s CEO John Milligan has since admitted that the company was “unable to have a good enough conversation with the payers.”
But Sovaldi and similar drugs remain appealing, offering the prospect of curing HCV and saving an enormous amount of money for healthcare systems in the long-term.
The Italian Medicines Agency (AIFA) recognised this, outlining an ambitious strategy to eradicate HCV infection in 6-8 years in Italy. AIFA realised it would need to approach this goal in a novel way, and inaugurated a new negotiating strategy involving transparent dialogue with patients, physicians, scientific societies and manufacturers.
AIFA instigated a procedure for the free supply of several anti-HCV drugs (including but not limited to Sovaldi) in extremely urgent cases. It then gradually included other patients in a staged manner – next was HCV-infected individuals enrolled on the list for liver transplantation with hepatocellular carcinoma in compensated cirrhosis.
Meanwhile, to ensure economical sustainability, the negotiated agreement included the de-listing of other drugs with the same therapeutic indications, for which the agreed cap limit for the last 24 months had not been already reached. The remaining resources from these de-listed drugs were redirected to cover the new treatments at no additional cost for the Italian national health system (until the original budget from the old drug would be reached, at which point a mandatory renegotiation for the new one would start again).
Several innovative HCV medicines are now reimbursed in Italy in a sustainable way that has been designed in collaboration with internal and external experts.
Payers: Evidence gathering and risk-sharing
The Cancer Drugs Fund (CDF) was first introduced in 2011 in England as a source of funding for cancer drugs that NICE had rejected or hadn’t reviewed, due to lack of cost-effectiveness. While it was good news for many cancer patients in England, costs spiralled out of control and the value of the CDF was questioned.
The CDF was redesigned in 2016 to be more sustainable and to collect data on how effective the drugs are. It means that a previously black or white decision-making process can now have shades of grey. For example, NICE can now approve a drug for a limited time only and have it paid for via the CDF while more evidence is gathered.
It also means the CDF can share the financial risk with industry. With its new financial control mechanisms in place, if the CDF has overcommitted its budget at the end of a financial year, pharmaceutical companies that have received CDF funding will be required to pay a rebate to NHS England.
These are useful mechanisms to have in place for expensive, curative medicines, such as Kymriah, the pioneering CAR-T cell therapy from Novartis – which demonstrated a 83% remission rate in children and young adults with B-cell precursor acute lymphoblastic leukaemia – and which is available through the CDF.
The newly designed CDF enables earlier access to potentially curative cancer drugs at lower financial risk, benefitting patients and the pharmaceutical industry.
Pharma: Performance-based rebates
When the price of Luxturna – a one-time gene therapy which can return vision to people blinded by inherited retinal dystrophy – was announced, analysts considered it fair. But coming in at $425,000 per eye, or $850,000 for most patients, Spark Therapeutics knew it was facing the unaffordability problem.
To overcome this, Spark outlined an innovative contracting model where the company would share the risk with health insurers by paying rebates if patient outcomes failed to meet specified thresholds. Efficacy assessments are made both in the short-term (30-90 days) and long-term (30 months), based on measures that are unique to Luxturna.
Whether Novartis, which has the ex-U.S. rights to Luxturna, will have success with a similar rebate scheme in Europe remains to be seen, but the company is working hard to finalize reimbursement deals in individual markets in 2019 and 2020.
Patients: Lobbying for interim access
Ever since Orkambi received EU approval for treatment of cystic fibrosis 2015, there has been a stand-off between the drug-maker (Vertex) and the NHS in England, with both sides unable to agree on a price.
This has left several thousand cystic fibrosis patients in England in limbo, with most unable to gain access to a potentially life-saving drug. Patients groups have been very active in trying to change this situation, and may be nearing a breakthrough.
The Cystic Fibrosis Trust for example, established Stopping the Clock, its own dedicated campaign to put pressure on the Government, NHS and pharmaceutical companies to ensure Orkambi and similar drugs reach the people who need them. It has proactively suggested access solutions – including allowing interim access and use of the UK CF registry to provide real-world evidence of the drug’s effectiveness.
Although no deal is in place at time of press, it is hoped that a breakthrough is in sight, with Vertex back at the table with NHS England and NICE.
Do we need a longer-term vision towards systemic change?
The kinds of solutions outlined in this article have been necessary to alleviate short-term access challenges, but they inevitably have limitations. They rarely involve all stakeholders – although the staged access for Sovaldi solution in Italy is a notable exception – and generally cover up the cracks in the short-term, rather than pave the way for long-term sustainability.
Of course, each situation is different, and the nature of the challenge somewhat defines the focus of the intervention (see diagram below).
Emergence of one-off, high-cost curative treatments calls for HC system-wide, multi-stakeholders long-term solutions
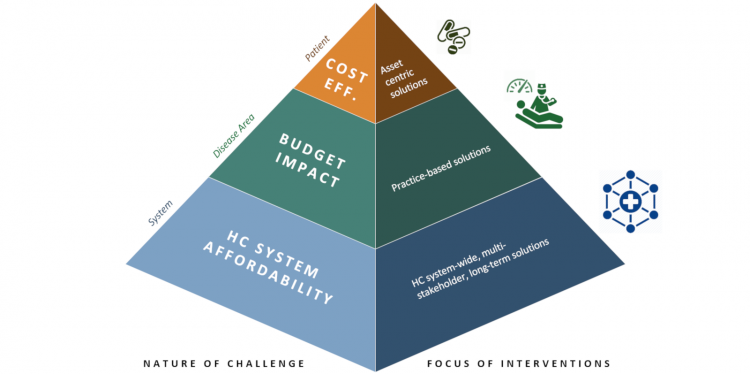
But with healthcare system affordibility as the key barrier to most one-off, high-cost curative treatments, the only sustainable solutions in the long term are likely to be healthcare system-wide, multi-stakeholder solutions. This is unlikely to happen organically; it requires vision and active oversight and management. Such a transformational journey requires a common agenda among all stakeholders and agreeing a definition of what constitutes fair pricing may be the first step.
“Fairness implies positive incentives/benefits for all stakeholders, including purchasers and those involved in the research and development and manufacture of medicines,” states the WHO. Is this right? How can we make this a reality with one-time cures?
These questions and more will be explored in Part 3 of this series.