Medical Affairs- The time for change is now
Medical Affairs is transforming into a key, central strategic function. Here Clifford Hall and Tanja Bosshard Becker from Executive Insight examine why Medical Affairs is uniquely placed to help pharma companies overcome the most pressing challenges in healthcare today.

In 2012, a McKinsey report predicted that by 2020, Medical Affairs groups would need to develop “a new set of competencies required to navigate the future healthcare landscape”.(1) That moment has already arrived. In the years since that report, the changes in the healthcare landscape have gathered speed and the importance of Medical Affairs has increased with it.
At the heart of the healthcare landscape changes is the shift from “price” to “value”. Health systems in Europe, as elsewhere, are under intense pressure to deliver better, more cost-effective care solutions. Fee-for-service models, associated with high-cost, high-volume care, are fast falling out of favour, and value-based systems linking payment to performance (and often shifting financial risk to providers) are more appealing.
As part of this trend, pharma companies are under pressure to prove the direct and indirect value of their medicines, devices and services to a wider, more diverse, group of stakeholders. Long gone are the days when it was enough to solely focus all efforts in communicating efficacy and safety to doctors. Regulators, policy makers, patients and, in particular, payers are now demanding a more complete picture on the potential value of new products.
While these changes call for closer collaboration between pharma and these stakeholders, the still relatively low trust towards industry can cause the opposite to happen. Regulatory changes increase level of control, oversight and restrictions on pharma operations – in particular on commercial functions.
Medical Affairs in the spotlight
All of these factors necessarily push Medical Affairs to the fore. Arguably, Medical Affairs has always been driven by external requirements – after all, it originally emerged due to pressures from regulators to separate medical and commercial functions. But now it has the chance to shift away from a supporting function to a central, strategic, customer-facing one, with an equal seat at the table with other leading functions such as Market Access and Marketing.
But why is the Medical Affairs function so well placed to help pharma companies address these environmental factors? Let’s examine them one by one.
1. Defining and delivering value
Medical Affairs is uniquely placed to work closely with all stakeholders to truly understand the challenges they face and to work as a genuine partner with them to find solutions, leading to improved patient care and creating value for all stakeholders.
These solutions may not always be related to the company’s products; sometimes it will be educational initiatives, disease management programs, real world evidence initiatives or any other activities aimed at improving a practice gap in the process of care. But by starting with recognising unmet needs in care and working towards solutions, companies can find ways to provide genuine value to those they serve.
An example for such solutions is the “Stent for life” initiative: Initiated by European cardiology societies “Stent for life” brings interventional cardiologists, government representatives, patient groups as well as industry partners together behind a common aim to reduce mortality and morbidity in patients suffering from acute coronary syndromes (ACS). 20 National Cardiac Societies and/or working groups or associations of Interventional Cardiology have signed a declaration that effective actions will be taken to fulfil the Stent for Life Initiative Mission in their country. Each member and affiliate is implementing an action programme to increase patient access to p-PCI.(2)
While that specific example underscores the benefits of early patient stratification and the use of biomarkers in clinics, there are many other ways to define value at an early stage in collaboration with stakeholders, leading to an increased chance of market access and, ultimately, success.
2. Stakeholder engagement
To define and deliver real value, it is vital to first establish meaningful collaborative relationships with stakeholders. Each stakeholder requires slightly different evidence or support - e.g. data, real world evidence, proof of quality of care, “beyond the pill” services - and pharma companies are increasingly looking to their Medical Affairs teams to gather the necessary evidence and share the information to each audience accordingly. For example, Lilly in collaboration with leading healthcare experts developed an education initiative called Fracture Liaison Implementation Program (FLIP). FLIP aims at supporting the implementation of Fracture Liaison Services (FLS) for secondary fracture prevention in patients suffering from osteoporosis. FLS is a coordinated multidisciplinary approach to patient care. The FLIP program has been endorsed by the International Osteoporosis Foundation.(3)
It is not just external stakeholders. Internally, Medical Affairs usually works across multiple touch points within an organisation, and therefore can serve as a central point to align various functions and franchises toward producing value for customers.
3. Regulatory pressure
A major element of establishing meaningful stakeholder relationships is establishing trust, and regaining trust is essential to counter regulatory pressure.
Medical Affairs teams are familiar with new regulations developed over the past several years and are generally perceived as fair balanced and credible sources of information; as such, they are well equipped to partner with stakeholders in a clear, transparent way that will ultimately help to rebuild trust. Taking leadership internally they can encourage other functions to follow that direction and find the right, evidence-based collaborative tone.
Indeed, as a facilitator that brings clinical and medical evidence together within the organisation and presents it to stakeholders, Medical Affairs can be the “unified voice” to communicate the company’s value proposition in a balanced and evidence-based manner.
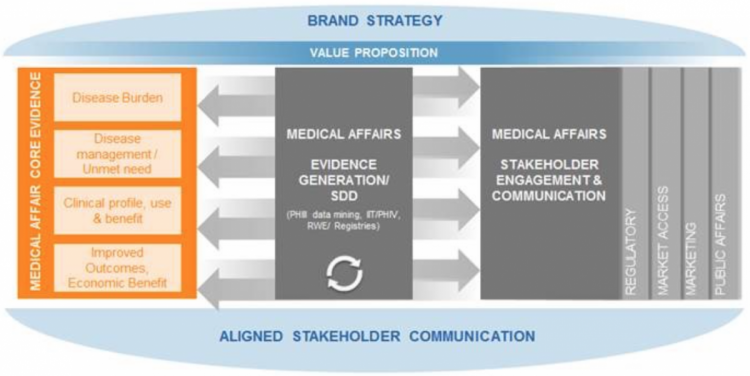
Image 1: Medical core evidence story as driver for an “unified voice” to stakeholders
All-rounders required
With the role of Medical Affairs changing dramatically, the necessary skill sets are changing with it. Medical Affairs professionals require a broader skill set than ever before encompassing, for example, customer engagement skills, an understanding of the regulatory environment, understanding of health economic evidence in helping to evaluate treatment options, and so on. It is no surprise that over 60% of pharma companies are “creating additional roles” to be able to communicate well with new influencers, particularly payers, and ultimately to help get their products to market.(4)
Identifying individuals with the right all-round skills – with both the deep scientific knowledge and expertise along with the business acumen and strategic thinking – is challenging. The breadth and complexity of the role could be one reason why we are seeing more outsourcing of Medical Affairs by pharmaceutical companies.(5) Indeed, 68% of global Medical Affairs groups now elect to outsource at least one sub-function, with medical information and medical publications as the two most frequently outsourced sub-functions.(6)
Medical education – leading by example
So what does this look like in practice? If we look at just one aspect of Medical Affairs – medical education – as an example, we can see an evolution from a tactical support team implementing educational programs to a core Medical Affair capability following strong disease-based strategy. Pharmaceutical companies have an ethical obligation to ensure that their products are used safely and effectively. Industry supported medical education should help address this imperatives and should address as well the Health care professionals educational needs, the healthcare system practice gap for the benefit of the patients.(7)
The result is that medical education can transform from being merely about transfer of product related evidence to actually impacting clinical performance. A lot of work in recent years has gone into ensuring medical education is linked with quality improvement. Measurement is shifting away from simple attendance or a time-based credit to metrics related to performance for successful learning, and there is an expansion of medical education to address population and public health issues.(8)
At the heart of the new wave of medical education is the question of trust. Proactive transparency is going to be paramount on all aspects of the program, including the role of the stakeholders involved in the creation and delivery of an educational program, ethical engagement rules followed and the potential benefit of its organisators.
The collaborative partnership model between industry and health care organizations is the preferred model in Europe to address jointly a well-defined educational gap involving shared responsibility between Industry and Health care organisation to develop educational programs. In addition, mirroring the overall trend in Medical Affairs, medical education is expanding to include activities designed for other key healthcare stakeholders beyond physicians, such as patients and payers.

Conclusion
The transformation seen in medical education in recent years is an example of the change in mind-set and approach that is required in other areas of Medical Affairs. With a strong value story and evidence to support it and a clear understanding of stakeholder needs, Medical Affairs can provide the backbone not only for all their own activities, but also for other functions. It can be the driving force behind a pharma company’s one unified collaborative approach to delivering value to its stakeholders.
References
- Evers M, Fleming E, Ghatak A et a. Pharma Medical Affairs - 2020 and beyond. McKinsey & Company. 2012
- http://www.stentforlife.com/
- http://www.capture-the-fracture.org/national-toolkits
- Current perspectives on the biopharma go-to-market model. FirstWord. January 2016
- http://www.outsourcing-pharma.com/Commercial-Services/Pharma-outsourcing-more-med-affairs-and-post-approval-work-say-experts
- http://www.reuters.com/article/nc-cutting-edge-idUSnBw285060a+100+BSW20140128
- Saxton M. A View from Industry: The Foundations of Future Commercial Support and a Call for Action. Journal of Continuing Education in the Health Professions. 29(1):71–75, 2009
- Balmer JT. The transformation of continuing medical education (CME) in the United States. Adv Med Educ Pract. 2013; 4: 171–182.










