Rare Diseases: The seamless Go-to-Market Model
How to do more with less and get ahead of the competition

Collectively, rare diseases are anything but rare. Combined, they represent a huge market; one that has been a major focus of interest and investment from the biopharmaceutical industry ever since the US Orphan Drug Act offered financial, legal and legislative incentives back in the 1980s.
The global market for orphan drugs is expected to grow at a compound annual growth rate of over 11% year-on-year, jumping from $138bn in 2018 to $262bn by 2024. That’s a staggering 22% of the overall prescription drug market.
There are over 7,000 known rare diseases, and over 30 million people living with a rare disease in Europe alone. Today, treatment exists for only 200–300 diseases. The scale of the potential – both for patients and for the industry – is huge.
So, what’s the drawback?
Well, there are a few. Some payers have become increasingly concerned at the increased market share of high-price orphan drugs, and now often seek to curb access or put more hurdles in place. Pricing and access can vary considerably between countries in Europe as each government decides the terms of reimbursement and prices that companies are allowed to charge.
Most rare diseases have been inadequately studied in the past, making clinical study design and execution challenging. The management of the patients themselves – who often have a reduced quality of life and, in some cases, limited life expectancy – requires sensitivity and careful management.
And crucially, there are challenges working in diseases with such few patients, who are often located over wide areas. In Europe, a rare disease is defined as a condition that affects fewer than five per 10,000 inhabitants, and is fatal or severely debilitating. Even in major European countries that have over 50 million inhabitants, this still means a total patient population of just a few thousand.
Identifying these patients – particularly for orphan drugs that are the first effective treatment for a rare disease – can be very difficult. By necessity patients are usually sent to a few specialist centres, meaning there are generally a few ‘cluster’ centres to focus on, but the lack of publicly-available hospital procedure classifications and case numbers makes it difficult to identify these centres. Biopharmaceutical companies are left with no choice but to engage with healthcare centres and professionals on the ground to understand patient pathways, which can be time-consuming and costly.
Top-down or bottom-up? Setting up your organisation for rare diseases
Because of the unique situation around each rare disease and the complexity of each launch, biopharmaceutical companies generally opt for dedicated organizations, even if they already have local affiliates in place.
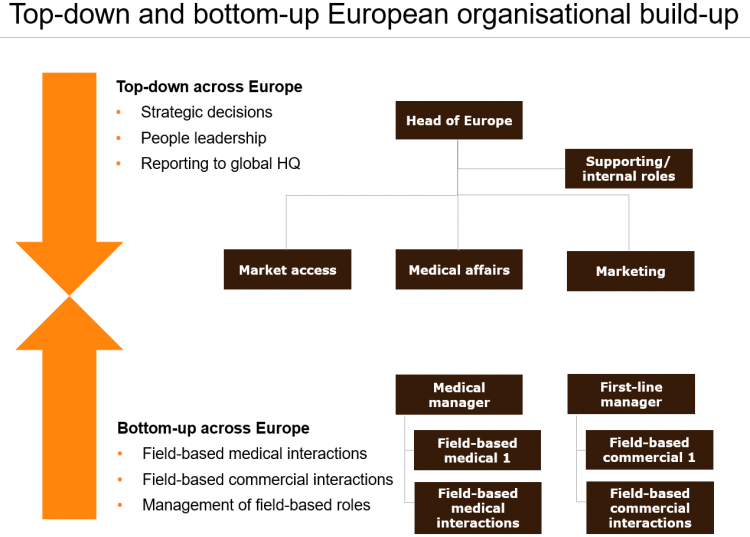
But what kind of model works best? There are two fundamental ways to build dedicated roles and headcounts across Europe: first, a top-down approach focusing primarily on strategic aspects and secondly a bottom-up approach, focusing on customer interaction.
The top-down organisational approach generally focuses on a few handpicked roles that can make the key strategic decisions. Typical European-level roles may include head of Europe, market access, medical affairs, marketing and other supporting roles, such as HR, finance, legal/compliance and so on.
Meanwhile, the bottom-up approach provides the on-the-ground knowledge and insights into rare diseases that are unavailable elsewhere. The bottom-up organisational set-up should focus primarily on both medical and commercial field-based interactions, and field-based market access where required, and the management of these field-based roles. During pre-launch situations, field-based medical roles should be located as close as possible to the key centres participating in clinical trials, enabling engagement with future key centres and European KOLs.
Identifying where dedicated resources are required
Both approaches have their advantages, so is there an optimal way for organisations to include elements of both?
The key consideration is around where you get your biggest value for investment. In practice, one field-based medical full-time employee (FTE) can engage with up to 15 centres, if he or she does not visit the centres more than once a month. In rare disease terms, that’s more centres than there usually are in a single country, and only the top five EU countries would have enough centres to justify a dedicated full-time member of staff. Mid-sized and smaller countries may need to share field-based medical employees.
Management of field-based staff is even more uneconomical. Even the largest countries struggle to reach critical mass to justify a dedicated role for people leadership, particularly with separated reporting lines between medical and commercial roles, let alone having two management layers with a Manager and a country head.
European Medical Managers can handle these tasks at the European level across several rare diseases. This is only really necessary when the number of FTEs grows and people leadership becomes a dedicated task.
It is a similar story with the top-down approach. Even the largest countries rarely need all the strategic roles in market access, medical affairs and marketing in place.
These roles can usually be handled at a European level across several rare diseases, particularly because rare diseases usually have similar standard of care, with well-connected Centres of Excellence and KOLs across the continent.
So, the key is to focus primarily on the field-based roles – this is where you will find the information and establish the relationships that could completely define your position in the disease area – but at the same time ensure a pan-European strategic support network is in place.
The optimal approach
The most effective and efficient rare disease biopharma organisations maximise the proportion of customer-facing FTEs, and ensure pan-European cross-functional decision-making between medical affairs, market access and marketing, and introduce as few layers as possible between these two (see diagram below).
So what would this look like in practice? In pre-launch situations, biopharmaceutical companies may have as few as one or two FTEs in each of the large EU five countries, which may also cover nearby centres and KOLs in neighbouring countries. They may also place additional FTEs at the locations of other top European centres and KOLs, resulting in around a dozen or less FTEs at that time. The field-based presence would increase further during launch, and may include Key Account Managers (KAMs) and, where necessary, field-based market access.
One consideration: if you implement a standalone model as a smaller biopharmaceutical company, you may need to plan flexible resourcing and outsourcing for some support at country level at certain times, for example when you are preparing an HTA dossier for local price submissions. If the model is part of an existing, larger organisation with those resources in place, it is important to establish and agree on interfaces between the two organisations.
Planning through principles
Of course, how you structure your organisation is a fundamental decision, so it is important to carefully consider your organisational design principles before making decisions. What is your company’s aspiration, now and in the next five years? Would you prefer to serve customers in Europe through a dedicated European rare diseases organisation or another way? What are your cultural priorities (eg customer-centricity, cross-functional collaboration and agility)? How will you prioritise your European customers? Will it be on their potential, their KOL presence, their status as a Centre of Excellence, or their affinity to you as an organisation?
When you have answered these questions, you can design your organisational structure with a combination of top-down and bottom-up approaches. Allocate strategic roles top-down across Europe, particularly for medical affairs, market access and marketing, and ensure cross-functional collaboration, ideally with a general manager role for Europe. Implement customer facing roles, field-based medical, commercial and market access (if required), and locate these in proximity to your prioritised customers. Crucially for cost-efficiency and agility, ensure you create the flattest management layer possible.
With all this in place, you should achieve the three key objectives for any go-to-market model: optimal stakeholder engagement, superior competitiveness and profitability.









