How to commercialise narrow indication products
With the blockbuster model wearing thin, the pharmaceutical industry has needed to diversify its go-to-market approach. Narrow-indication products are becoming a more popular option for big pharma, with benefits such as smaller and less expensive clinical trials, smaller customer bases that can be covered by a reduced field force, a streamlined approval process and a higher likelihood of being first in class. But what is the optimal way to bring such products to market?

Big pharma is used to doing things in a tried and tested way, and companies often utilise the traditional affiliate-based model to commercialise its products worldwide, regardless of the nature of the customers and economic potential of the drug. While this method has been successful for the blockbusters and mass-market products, some of its benefits become weaknesses when applied to narrow-indication therapies.
For example, the comprehensive nature of the affiliate model - arming each country with the personnel, budget and autonomy to launch the product nationally -becomes an inefficient and wasteful way to reach a much smaller number of stakeholders; the proverbial sledgehammer to crack a walnut. Efforts are duplicated unnecessarily in each country, wasting time and money and resulting in a less compelling offering to customers. The country silos also hinder effective knowledge and best practice sharing between countries, while smaller affiliates don’t have the critical mass to dedicate specialised resources. Highly specialised physicians are much better served by engagement with international events, projects and programmes, which develop their regional or global networks.
Similarly, from an operational perspective, mass-selling products, delivered to large and less-specialised customer groups, can benefit from large affiliate organisations at a local level. These affiliate organisations typically have profit and loss (P&L) responsibility, a high degree of independence and a country-specific approach to market. This is not optimal for narrow- indication therapies, where limited sales potential dictates the need for efficiency in order to reduce operational expenditure. Country boundaries are less important and global/regional teams need the flexibility and authority to easily deploy consistent strategies, plans and initiatives across geographic boundaries, with the field forces focussing on implementation in their areas.
There is, therefore, a need for big pharma to utilise a more innovative approach to market narrow-indication products, and the lower the economic potential of the drug (due to small patient numbers), the more likely that an innovate model will be a strategic imperative for profitable commercialisation.
What is the blueprint for success?
Perhaps most importantly, effective models for narrow-indication products should be designed to reflect the limited numbers of stakeholders involved, and to consider country boundaries as a less important factor.
Narrow-indication therapies are generally used by a small minority of healthcare professionals, often concentrated in a few of the larger hospitals. Working with a small number of high-value centres and customers requires a very high quality and personalised customer experience. Only a small number of expert field force personnel are required and they do not necessarily require a national infrastructure to support them.
The highly specialized customers have specific needs. These include ad-hoc, and sometimes urgent, discussions of patient cases with leading global or regional centres that have extensive product usage experience, and the need to share clinical experience across geographical boundaries, in particular leading countries sharing with less experienced countries. This point is particularly important, because without a significant number of local peers using the treatment, physicians are reliant on international networks of peers to discuss patient cases and education on the latest developments in diagnosis, treatment and management.
Creating a regional (e.g. pan-European) organisation
So how can large pharmaceutical companies service such requirements effectively and efficiently? Enter the centralised commercial model. Centralised models can be global or regional, but for the purposes of this article we will refer to it as the pan-European model.
A pan-European model requires the establishment of a central European organisation with the specific remit of commercialising the narrow-indication product. The organisation has two main priorities; the first is bundling the product with very high value-adding services to physicians and payers alike. The second is increasing efficiencies and effectiveness by centralising activities wherever possible. All activities that do not require deep local market knowledge are centralised, leaving only field roles such as key account managers, medical science liaisons and market access managers in the countries./
Assessing all team responsibilities (figure 1), provides a strong basis for designing the teams that will deliver the commercial model.
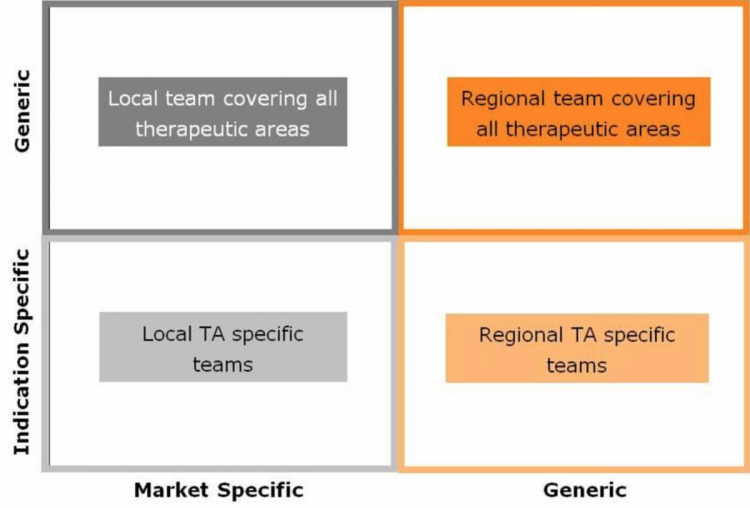
Priorities are decided centrally at the European level, with all commercial operations personnel reporting into a single centralised organisation. Hospitals and customers are segmented centrally, and field forces sizes are determined based on the number of target hospitals in each geographical area (not necessarily by country). Clinical research is prioritised centrally, sponsoring the most medically relevant studies irrespective of geography. Strategies, services and projects are developed centrally and implemented in the geographies. A light back- office support group (HR, finance, compliance and so on) supports the central organisation.
In order to win the trust of these highly specialised customers, the sales approach is highly customer-centric, with an ongoing focus on generating relevant new scientific data and improving patient health outcomes by optimising the patient pathway. Customer- facing sales involves a much smaller and more scientifically sophisticated field force, who despite being geographically widely spread, are able to stay continually connected due to modern technology.
Gaining internal buy-in
From our experience of implementing this model, it is vital to gain buy-in throughout the organisation. You must secure unwavering support from the top executives for the initiative, from the conception of the idea through the lifespan of the organisation.
high degree of organisational change must be guided by a strong communications plan, which has the ‘win-win’ message at its heart for all involved.
Crucially, the company affiliates must understand that the approach is mutually beneficial, and must be brought onboard with the plan early on. While the centralised pan- European model is run independently, the affiliates will be providing local support in areas such as regulatory, market access and legal. With the pan-European organisation commercialising the products that do not fit with an affiliate model, the affiliates will be able to focus on their broader indication and primary care products.
If the channels of communication are not open, the centralised organisation can run into trouble with the affiliates. One of the main reasons for initiating a Pan-European organisation is for narrow indication products that are unprofitable – as such, the affiliates are initially happy to have the unprofitable and problematic products off their books. However, once the centralised approach has reaped success and the products start returning a tidy profit, the affiliates become interested again, potentially causing a destabilising effect. In addition, affiliates may feel threatened that this new and successful model may spread to take on other specialty therapeutic areas currently under their remit. There are other potential challenges. For example, as the organisation evolves, new teams, and positions are likely to be created, and existing ones will change. This poses a problem for HR, who will need to ensure career progression remains smooth for people moving back to the affiliate organisation, and that incentive schemes remain fair between the affiliate sales force and their sales team.
Finally, this will be a highly complex and risky migration. The guidance of an experienced partner has proven to be extremely beneficial in terms of reducing time-to-market, creating the right organisation design, identifying the ideal positions and ensuring seamless implementation, specifically for your narrow- indication therapy’s situation.
Reaping the benefits
In our experience of implementing pan- European and global centralised models, our customers have achieved consistent benefits. Not only is a pan-European model much more effective at serving the specific needs of these small, highly specialised customer groups, it will do so at a dramatically reduced cost, capitalising on the fact that the very small field force requires no local infrastructure, and eliminating all duplicitous efforts.
The centralised approach integrates physicians across country borders, providing physicians with access to Europe’s leading centres, facilitating education and best-practice sharing and improving patient outcomes.
From the pharmaceutical company’s perspective, it should develop stronger relationships with European-level KOLs, societies, payers, governing bodies and regulatory bodies. In addition, the organisation can be up-scaled easily to take on new indications and new drugs, thus introducing further efficiencies through economies of scale.
The centralised model clearly seems to be the best option for commercialising narrow indication drugs to small specialised customer groups. From a business perspective, this model is likely to maximise profitability no matter how small the peak-sales expectations of the product.



