Organising for Networked Healthcare (Series Part 3)
In recent years, the healthcare environment has become increasingly networked as a growing number of interrelated stakeholders are gaining decision-making power in the prescription process. The authors argue that companies that do not adjust their organisations to these changes will loose ground to the competition. These companies will find it increasingly difficult to support their traditional target customers and will not be able to address the dynamic needs of important nonprescribing stakeholders.

The paper provides an organisational design framework and ideas of how companies can re-organise their commercial operations to remain viable in the future. Two cases present a practical understanding of innovative organisational design.
Journal of Medical Marketing (2007) 7, 6–17. doi:10.1057/palgrave.jmm.5050062
Introduction
At a large pharmaceutical conference in March 2006, one of the key note speakers stated that everybody knows that the ‘share of voice’ model is out of date, but nobody wants to take the first step of radically reducing the size of the salesforce, risking the loss of market share. A wave of consent went through the audience. In the subsequent breaks, one could see groups of pharmaceutical leaders discussing the situation and complaining that not enough conference time would be spent talking about the real challenges of the industry. While it is true that pharmaceutical companies see their margins shrinking and their customers complaining that sales representatives do not add any value, salesforce sizing alone will not solve the fundamental challenges behind the fading ‘share of voice’ paradigm. It seems pharmaceutical companies are, however, simply planning to tweak their pure ‘size sells’ strategies by improving targeting. As a result, they will try to apply the same size-related logic, largely responsible for creating the problem, as a solution to the problem — the only mindset shift being that now ‘margins matter’.
This paper, which is the third in a series of four dealing with the challenges of the networked healthcare environment, presents ideas on how pharmaceutical companies can successfully organise their commercial operations. The underlying assumption is that the pharmaceutical stakeholder environment is becoming increasingly networked and that companies can address many of the current challenges by fundamentally reorganising their commercial operations.
Based on front line experience, the paper presents ideas for future organisational models in the form of organisational requirements (ie focus, learning, innovation and implementation) and core dimensions of organisational design (ie strategy, people, culture and structure). These ideas are expressed in two models that have been developed based on research of highly organisationally innovative European pharmaceutical companies. The two models are labelled the Competence-Based Organisation (CBO) and the Mirroring Organisation (MO).
For purposes of delimitation, it is important to note that it is not within the scope of this paper to provide a methodology on how to develop the organisational design for pharmaceutical commercial operations. It should also be emphasised that there is no ‘one size fits all’ design that would serve all pharmaceutical companies. Nevertheless, it is necessary to start thinking about alternative types of design models that go beyond the current standard of sales, marketing and medical functions; models that provide ideas on how pharmaceutical companies can organise their commercial operations to remain viable in the future.
The situation today
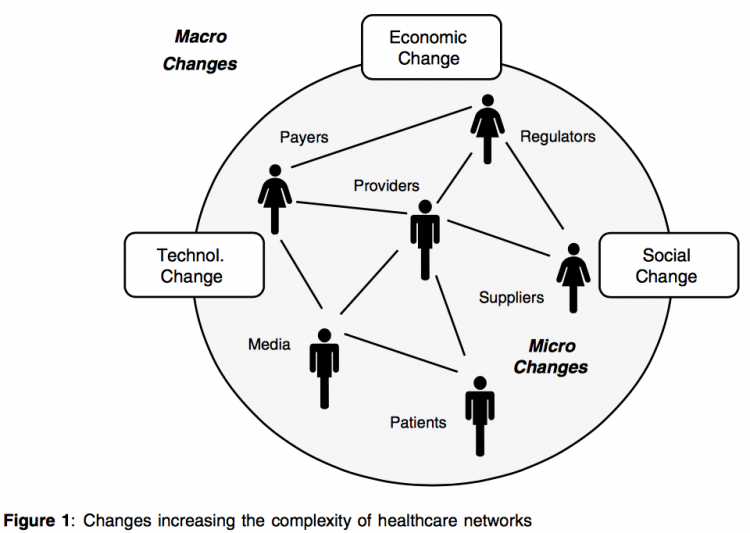
In recent years, the healthcare environment has started to change fundamentally and is becoming increasingly complex. This complexity is driven by macro- and micro-changes inside the healthcare market (Figure 1).(1) These changes are making the healthcare environment an increasingly networked and thus complex arena in which to operate.
The changes within the healthcare networks are driven by two forces. First, there is an increasing influence on prescription decisions by a number of new stakeholders (eg new health authorities and new types of opinion leaders such as nonprofit organisations) and existing stakeholders (eg governmental bodies and formulary committees). Secondly, there is a rapid emergence of new, highly dynamic, relationships between the different stakeholders. GPs and specialists are basing their prescription decision making on an increasing variety of factors, opinions, information sources and interests.The pharmaceutical sales representative is just one of many players with whom physicians have professional relationships, and no longer have pre-eminence.
To demonstrate how the relationships between stakeholders are changing, let us examine the case of a large German hospital centre.The centre started to network with GPs, peripheral hospitals and ambulance services, all involved in the treatment of cardiology patients, in order to develop and implement a joint treatment guideline.To prepare the ground for the network, the chief cardiologist of the centre (ie the ‘network leader’) started to discuss treatment alternatives with insurance companies and contacted potential network members.The discussions with insurance companies were important due to their ability to accept or reject treatment alternatives. The economic impacts were carefully assessed to avoid penalising any of the parties involved. Based on the results of these discussions, several facilitated network meetings were held to develop and implement a commonly agreed treatment guideline. Within the first year, the network produced a significant improvement in patient care quality and an overall reduction of healthcare cost.(2)
But where were the representatives of the pharmaceutical industry in this example? Even if sales representatives had noticed that an important customer was about to form a ‘guideline network’, they most likely would not have been able to play any part in this development. In fact, experience has shown that most commercial operations are not capable of addressing such developments, largely due to internal rigidities.Would marketing, sales or medical own the programmes supporting the guideline development? Would the competencies needed to perform the support come from one function alone or would cross-functional competencies be required? Who would have the incentive to coordinate and drive the corresponding activities? These are the kind of questions that address the issue of organisation.
Organisational requirements for ntework centricity
Today, there is a widely spread awareness among pharmaceutical leaders in Europe that the changes described in the previous section are taking place, and that they will have fundamental implications on the way pharmaceutical companies need to organise their commercial operations. Companies that do not adjust their organisations will increasingly loose ground to the competition with respect to market share and sales performance.The reasons for this are two-fold. First, these organisations will find it difficult to support their target customers in becoming more successful in the increasingly networked environment (eg the ‘network leader’ in the previous example). Secondly, these organisations will not be able to access and address the dynamic needs of important nonprescribing stakeholders (eg insurance companies and ambulance services). Consequently, one of the most important questions that pharmaceutical leaders need to answer is which requirements their organisations need to meet in order to remain viable in an increasingly networked environment.
As outlined in the previous paper in this journal’s networked healthcare series, one critical organisational requirement is the ability to develop an in-depth understanding of the networked environment.(3) The paper outlined the concrete steps on how a pharmaceutical company can identify, map and interpret influence relationships between stakeholders in the healthcare market. A solid network understanding is a prerequisite for the organisation to be able to focus on the growing number of strategically important nonprescribing stakeholders.
Understanding local networks and the different types of influencers in a network is, however, of limited value if the marketing and sales operations continue working in the traditional, functionally separated, way. To continue the example of the ‘guideline network’: it does not help the sales representative much to know that their most important customer is starting to form a network if they cannot act upon this information. In order to gain access and create value for such networks, the sales representatives need to leave their traditional role as ‘information providers’ and evolve into ‘network enablers’. This switch might be highly challenging as it requires a mindset shift and new skills from individuals.
From the broader perspective of commercial operations, the challenges are equally fundamental. Commercial operations need to develop new organisational competencies, services and delivery capabilities to actively facilitate the customer networks. In this paper, organisational competencies are defined as a ‘combination of complementary skills and knowledge, embedded in a group or team, which results in the ability to professionally execute one or more critical processes’. Hence, organisational competencies are something different than the sum of the competences of individuals. In addition, these competencies are considered strategic if they allow a firm to differentiate itself from the competition.(4,5)
For instance, a guideline network would need support both in event management (eg organisation of a kick-off event) and online interaction (eg online platform for virtual interaction and access to valuable information resources, such as guideline examples).The competencies needed to develop and implement such services are not likely to be found in one function alone.The most critical competencies, such as the ability to professionally support customer networks, would typically reach across such functions as medical (eg medical content), marketing (eg programme development), customer service (eg meeting and event logistics), IT (eg collaboration technology) and sales (eg local operative assistance).
The example above illustrates that the changes in the healthcare environment are likely to call for fundamental changes in the way pharmaceutical companies organise their commercial operations. In particular, pharmaceutical organisations need to boost their ability to learn and innovate across functions, and rapidly get new services and solutions out to the market.Table 1 summarises four critical organisational requirements that commercial operations need to meet in order to address emerging stakeholder needs, and successfully cope with the challenges of the dynamic networked healthcare environment.

Reviewing the organisational requirements above, it becomes apparent that designing the right organisation is not an academic pleasantry, but rather a crucial task for enabling the creation and delivery of added value beyond the supply of drugs to the healthcare network. Ultimately, the new design will increase patient value, which is the key challenge within the healthcare arena today.(6)
Design dimensions
Organisational design is widely recognised as a major determinant of organisational performance and competitive advantage.(7) Simplistically, the design of an organisation should match the distribution of resources, authority and information as closely as possible to the purpose the organisation seeks to achieve. It provides a formal context that shapes the behaviour of the people within the organisation. In turn, it is the behaviour of people that brings the design of the organisation to life and determines its effectiveness.(8) In other words, designing the organisation to address the challenges of the environment entails more than drawing the boxes and lines of a new organisation chart. Changing organisations to ensure survival in dynamically changing business environments means changing organisational culture — the values, orientations, behaviours and leadership style that shapes the ‘us’ versus ‘them’, the ‘right’ versus ‘wrong’ and the things that are important versus those that are not.(9–13)
The structural components of an organisation (roles and responsibilities, reporting lines and supporting systems) represent a necessary, but certainly not sufficient, dimension of the overall organisation design. Business practice (not only in the pharmaceutical industry) shows that the so-called soft dimensions of ‘people’ (capabilities and skills) and ‘culture’ tend to be neglected when designing organisations.They are difficult to grasp in tangible ways and to ‘engineer’ into blueprints for processes, structures and systems. They, however, tend to be at the top of the list of reasons for failure. For instance, there is a great deal of evidence that reconfiguring tasks into cross- functional teams of sales, marketing and medical members does not automatically result in the intended collaborative behaviour, unless other aspects such as leadership behaviour and organisational culture are changed as well.(14)
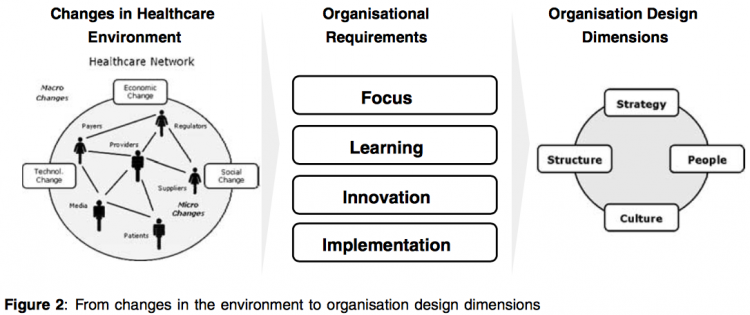
The point is that all critical design dimensions need to be aligned and balanced to design an effective organisation.The design dimensions considered in this paper are strategy, structure, people and culture.(15) Figure 2 provides an overview of how changes in the healthcare network result in new organisational requirements and related changes in organisational design. The combination of organisational requirements for network centricity and organisation design dimensions serves as the conceptual basis for the organisation design of pharmaceutical commercial operations (see Table 2). What should the strategic, structural, people and cultural dimensions of the organisation look like to fulfil the organisational requirements of focus, learning, innovation and implementation that are critical to meet the challenges of a changing healthcare network?
Design solutions for organisations
As stated in the introduction of this paper, each pharmaceutical company has its own individual context for which no optimal ‘one size fits all’ solution exists. Nevertheless, models can provide highly relevant ideas if combined with personal experiences and related to the specific organisational situation at hand.This section presents two such models that were developed based on first-hand observation of European pharmaceutical companies.The models are labelled the CBO and the MO.While the CBO is being used in a context of secondary care and the MO in a context of primary care, both models are examples of organisational innovation that are applicable to commercial operations regardless of their product focus.
The CBO specifically addresses the increasing organisational need to systematically develop and leverage organisational competencies (eg competence in hospital quality management or reimbursement systems) that focus on innovations for targeted customers and customer networks.This focus makes sense due to the relatively high margins and small, specialised group of target customers.
At the very heart of the CBO are the processes of competence development and innovation, enabled by so-called ‘competence teams’.These teams are composed of members from different functions, responsible for the development of strategic competencies and their transformation into solutions (eg services, applications, tools). Despite a stronger alignment with the business strategy and a clearer organisational responsibility to transform competencies into solutions, competence teams are related to the concept of ‘Communities of Practice’.(16)
Another critical aspect of the CBO is the strong integration of selected customers in both competence and solution development.The cooperation goes far beyond traditional ‘advisory boards’ that simply provide feedback. For instance, highly interactive workshops are organised to draft a shared vision of a potentially radically different future, and jointly develop solution ideas that aim at making all parties involved more successful. From the perspective of the CBO, customers can fulfil three distinct roles within this setting.They can be viewed as ‘information sources’, ‘co- creators’ or ‘users’. As an ‘information source’, the role of the customer is to exchange information and knowledge about solution ideas and concepts. As ‘co- creators’, the customers are involved in the creation of new solutions. Finally, as ‘users’, customers are involved in solution testing and piloting. In fact, the strong integration of customers into the CBO, and vice versa, strongly blurs the boundaries between the CBO and its environment, shifting the power from the firm to the community.
Despite the blurred boundaries, the CBO still needs a structural organisation. Based on the assumption that the needs of physicians are not determined by their nationalities, the CBO tends to structure across countries (eg Pan-European organisation). A cross-border organisation facilitates the leveraging of local experiences (eg customer projects) and networks customers with similar interests across borders (eg support of a Pan-European registry). In addition to the leveraging of experiences, the competence development and innovation processes require coordination. For this purpose, the CBO typically has a dedicated team responsible for the support of all parties involved in the competence development and innovation process, and a governance function responsible for prioritisation of investment in innovations (eg with respect to which innovations to pilot and implement).
The CBO design attracts and requires people with a particular set of skills and capabilities. For instance, employees must be willing to share knowledge and experiences openly across functional and geographical borders, and possess the ability to work within dynamic competence teams.The concept of the CBO is based on the insight that employees (often hidden in affiliate structures) and unidentified or inaccessible customers often hold specific knowledge that could create substantial value if shared and transformed into solutions. According to this view, firms have the opportunity to open up the ‘treasure chest’ of knowledge by enabling knowledge sharing between their employees and customers.
The design of the MO is well suited to implementation in individual countries with a relatively large portfolio of prescription products across several therapeutic areas and a wide range of influential, prescribing and nonprescribing stakeholders.This emerging design type specifically addresses the increasing importance of the nontraditional stakeholder groups, and embraces a network-centric approach by establishing dedicated customer-departments for all critical stakeholder groups.This enables a strong focus on the relevant members of the healthcare network — one of the strategic organisational requirements for addressing the networked environment.
This type of organisation design reflects or ‘mirrors’ the nodes of the network. The focus on the influential stakeholders of the network is coupled with a completely different approach towards these customers: fewer sales representatives make fewer but longer visits that are focused on creating real value for customers and building stronger relationships.The external focus on different stakeholders is complemented by an internal, cross-functional collaboration process between marketing, sales, medical and other supporting functions, to share lessons learned, develop and efficiently deliver innovative programmes and solutions for the distinct stakeholder groups.
The most critical challenge for this type of organisation design lies in the cultural dimension.The new way of interacting with traditional and nontraditional customers (listening and learning, rather than pushing product details), as well as the cross-functional, collaborative innovation process require distinct new values, mindsets, behaviours and individual capabilities.The emerging results of this design type are, however, very promising: improved sales with a smaller salesforce. The point is that this is only made possible by organising and doing things differently; not by keeping the same sales approach and simply reducing the number of sales representatives.
Both emerging organisation design models adapt to the specific micro- and macro-changes of the healthcare environment, and fulfil the critical organisational requirements of focus, learning (from and with customers), innovation and implementation.
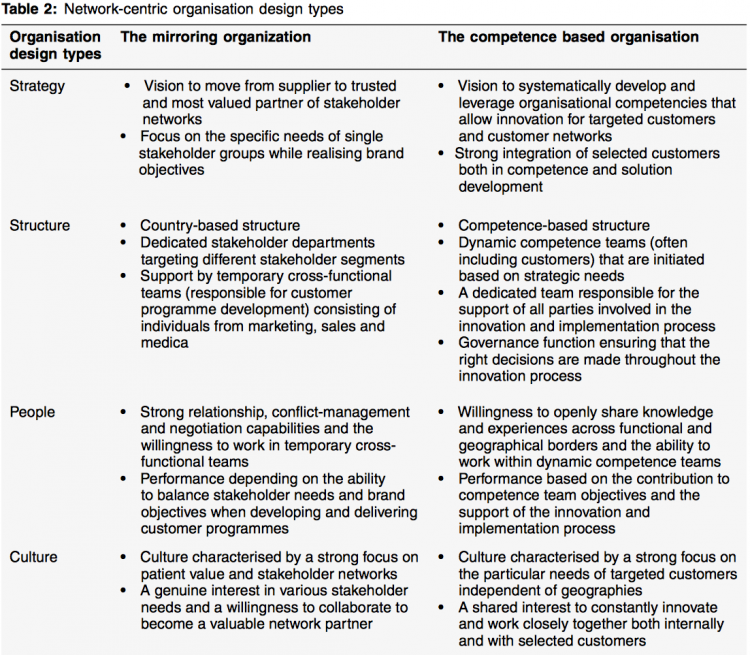
An ideal pharmaceutical organisation fully embraces the dynamic networked environment and has specific network- centric features built into all core dimensions of its design.Table 2 gives a summarised overview of the network-centric features of the two emerging organisational design types.
Both organisation design types embrace specific network-centric elements of the healthcare environment that make them quite distinct from the traditional functional organisation of pharmaceutical commercial operations.What stands out in both designs is the newly acquired ability to learn about the needs and dynamics of the network stakeholders, and to subsequently transform these insights into services that are of true value to the customers. Of course, pharmaceutical products remain, and the services and offerings such as compliance programmes or patient outcome data measurements are largely related to the company’s products. But these new services go well beyond the pure product-centred messages.
It needs to be emphasised again that there is no ‘one size fits all’ design solution, and that the above emerging design types are only examples indicating the general direction for designing a customer-centric organisation.The important point is that all critical requirements and design dimensions should be addressed in the organisational design.
In order to gain a more in-depth understanding, two cases are presented in Boxes 1 and 2. Box 1 provides a real- world example of a CBO called H-Care. Box 2 features the case of P-Care that summarises the essential elements of a number of presently ongoing organisational transformation projects towards an MO design. Both cases are based on long-term professional consulting engagements of the authors. In response to the environmental market challenges of difficult access to prescribing doctors, ineffective field visits, newly emerging stakeholders in an increasingly networked healthcare environment and a public perception of the industry being a main driver of healthcare costs, several pharmaceutical companies have started to experiment with new organisational designs that reflect or ‘mirror’ more of the customer environment. Such attempts can be seen in initiatives where companies are installing ‘voice of customer’ departments, encouraging customer input to become part of product plans, establishing regional brand teams or setting up a number of specific customer departments. Owing to client confidentiality and the mix of options available, the following ‘ideal case’ combines the essential elements of a number of ongoing, real life organisational transformation projects towards a ‘mirroring’ organisational design.


Conclusion and outlook
Galbraith notes that ‘one of the primary barriers to converting to a customer- centric organisation is the belief that a company is already customer-centric’.(17) And indeed, pharmaceutical commercial operations do claim to be customer- oriented, and the individual sales representative or marketing officer certainly will make this claim with full commitment.The key question is, however, whether the organisation is enabling this customer-centricity by focusing on the right stakeholders and networks and taking full potential of its people and competencies or whether the driving rationales for action and behaviour are embedded in discrete functional budgets and logic.
In this paper, the point is made that, in the changing healthcare environment, pharmaceutical companies need to reorganise their commercial operations. The competence-based and mirroring models that were explained represent solutions on how to adapt to an increasingly networked and dynamic market. ‘The organisation’, often perceived as the necessary evil of bureaucratic structure, is proposed as enabling platform to unleash the potential of available resources. It should enable to better understand the needs of the important stakeholders and allow people across organisational borders (including customers) to systematically share knowledge to develop innovative and value-creating solutions for the healthcare network such as supporting providers developing treatment guidelines and improving patient outcomes. These value- creating solutions will contribute to the much needed improvement of healthcare systems across Europe and will lead to the desired integration of pharmaceutical companies into the healthcare network and into society overall.This specific issue will be the focus of the following and final paper in this series on networked healthcare.




