The Network is the Customer (Series Part 1)
What will the marketing and sales organisation of a typical pharmaceutical company look like in 5 years’ time? What activities will they be conducting? Who will be their customers? Crucially, how are they going to address the challenges the industry is facing, such as declining physician access, limited customer loyalty, downward pricing pressure and low levels of public trust?

Indeed, these problems are largely the result of the business model favoured over the past two decades by the industry, namely an excessive focus on prescribers and one-way, product-centred activities. Introducing a series that proposes a new go-to-market approach, this article will explain the concept of networked healthcare, demonstrate how the industry is becoming more networked and outline the implications for pharmaceutical companies.
Journal of Medical Marketing (2006) 6, 165–171. doi:10.1057/palgrave.jmm.5050038
The situation today
The healthcare market has always consisted of a number of interconnected players: general practitioners, specialists, nurses, pharmacists, health insurers, patients, to name but a few. Without fully ignoring the other stakeholders, the prescribing physician has been the traditional centre of attention of pharmaceutical companies’ strategy and interventions. Consistent with this focus, companies have over the previous decade massively increased the number of sales (1) representatives, whose main purpose is to deliver a product-focused message. The so-called ‘arms race’ provided first movers with a significant advantage. Over time, the followers have caught-up, leading to a stalemate (and some would venture, a climb-down). Marginal returns on the sales force are down, and the doctor’s waiting room is full of sales representatives. The product-driven ‘share of voice’ model is in need of an overhaul.2 Meanwhile, non-prescribing stakeholders, with a completely different set of needs than physicians, have been gaining influence on prescribing decisions.3 Recognising the emergence of new influencing groups, pharmaceutical companies have set up dedicated sales teams or roles, alongside the traditional primary and secondary care teams. And yet, to a large extent, pharmaceutical companies have failed to develop go-to market models that simultaneously address multiple stakeholder types and bring customer needs back into focus.
Defining a healthcare network
To understand the dynamics of this changing environment, we turn to the concept of social networks. A social network is a structure made of nodes, that is, individuals, and ties, who connect the nodes between each other. Social Network Analysis emerged in the 1930s as an academic discipline, rapidly proposing a variety of tools to map and measure the dynamics of interaction within networks. Research across a range of disciplines has since demonstrated that social networks operate on many levels, from personal relationships within families up to the level of nations, and play a critical role in determining the way problems are solved, organisations are run and the degree to which individuals succeed in achieving their goals.(4)
Now consider the healthcare environment.The nodes of the network are primarily individuals, such as pharmacists, hospital administrators, physicians, nurses and patients. Taking network analysis a step further, the nodes can also be organisations, such as governmental bodies, formulary committees, health insurers and pharmaceutical companies.The common denominator shared by these nodes, both individuals and organisations, is that they all have a direct or indirect influence on patient health, from prevention through to provision of care.
The ties, or connections, between the nodes, can be of different types. They can, for example, be contractual (eg a physician becoming a preferred supplier to a private insurance), consist of a physical flow (eg patient flows) or of a social nature (eg general practitioners (GPs) influencing each other at a local level).The connections can also be qualified in a variety of ways: for example, the frequency of interaction, the duration over time, the strength of the association or the degree of influence between the nodes. Influence, which can in turn be measured in terms of formal power, reputation and number of patients impacted, is of particular interest to pharmaceutical firms, who aim to drive sales by influencing prescribers.
To summarise, we define a healthcare network as a group of inter-connected stakeholders who have a direct or indirect influence on patient health. If healthcare networks have always existed however, they are becoming more complex.This complexity is driven by changes in the network environment (ie macro-changes) and changes within networks (ie micro- changes) as illustrated in Figure 1. In the next sections, we will explore these factors in more detail.
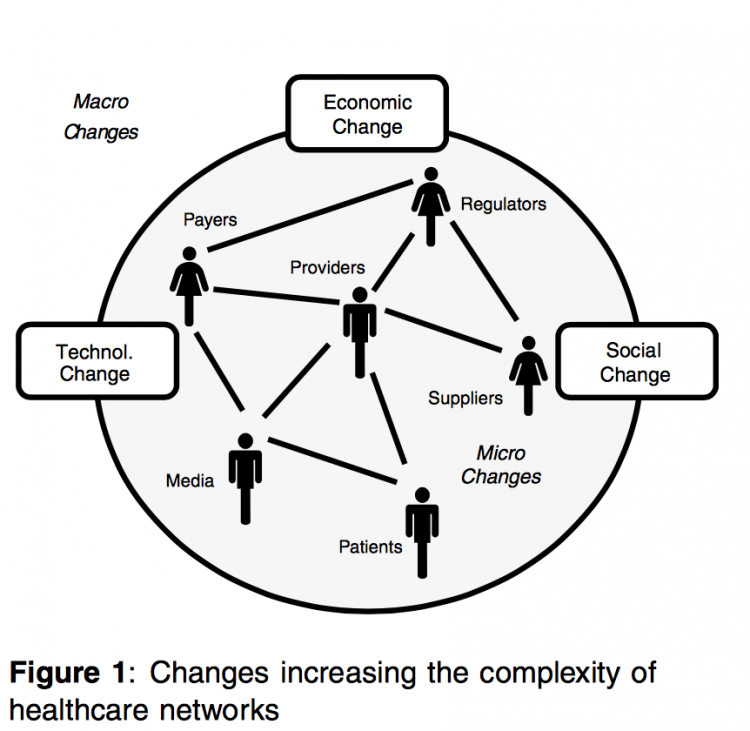
Enviromental change
A number of changes in the environment impact healthcare networks as a whole.
These changes essentially fall into three categories we call macro-dimensions: economic, technological and social. Together, they have a profound effect on the different stakeholders in a healthcare network as well as on the interaction and relationships between the stakeholders.
Economic change
Total healthcare costs in Europe and in USA have increased in recent years, prescription drugs being one of the most rapidly growing components. Increased use of drugs has affected the growth in prescription drug spending more than rising prices. Important factors contributing to the trend are the ageing of the population, increased prevalence of chronic diseases and obesity, improved diagnosis and treatment of treatable illnesses, improved therapeutic agents and finally increased compliance to treatment.(5)
Grappling with increasing healthcare bills, insurance companies and national healthcare payers are exploring ways to save costs and raise efficiency. A good example of such initiatives is the progressive establishment of Diagnosis- Related Groups (DRGs) in various countries across the European Union. With the aim of managing, controlling and reducing spending by classifying patients into groupings based on common diagnosis characteristics, DRGs are driving the clustering and specialisations of hospitals. Successful DRGs are also resulting in a more integrated web of professional services, as patients are treated by a tighter network of GPs, hospitals and pharmacies. In one case in Stuttgart, Germany, high street pharmacists are working closely with the hospital to establish proper medication dosages.The pharmacist can then act as a primary contact point for patients after they leave the hospital, answering questions about the medication and reducing the hospital return rate. A more integrated network enables an improvement in patient care quality and an overall reduction of healthcare cost.
Social change
Societal changes are also leading to an increase in network complexity.The high- profile media exposure of industry failures, such as the Cox-2 crisis, has dented public confidence in pharmaceutical companies, leading to increased industry regulation. Better-informed patients, with higher expectations of treatment outcomes, have less trust in their physicians, calling their judgment to account. As a result, decisions regarding disease prevention, management and treatment are more likely to be conducted as a collective effort between the patient, physicians and various other network stakeholders.
Technological change
Technology, and more specifically the internet, has also contributed to further integration of healthcare networks: as an information source, a communication tool and a transactional channel. In the case of healthcare professionals, databases such as Medline and Pubmed allow quick access to a growing amount of information and opinion sources, as well as up-to-date research results. In addition, physicians are beginning to use online technologies (eg collaboration platforms such as Doctors.net.uk or the Cochrane Collaboration) to develop online networks with peers.These peer-to-peer networks have the potential to allow healthcare professionals to improve both the quality and cost efficiency of patient treatment.(6) Finally, technology is enabling an increase in interactions between healthcare professionals, for example, through online referrals, electronic medical records access and electronic prescription transfer.
But just as the internet opens up medical information for physicians and healthcare professionals, it also provides patients better access to medical information and allows them to become more proactive in the drug decision and treatment process. It allows patients to communicate with each other and create large patient groups with the power to influence healthcare policy.
Mobile technology has also increased the interaction between different network stakeholders. Text messaging is, for example, used to enable the physician– patient interaction (eg appointment reminders), spread medical information (eg the World Health Organisation’s campaign to control tuberculosis, malaria and human immunodeficiency virus) and drive compliance (eg medication regime reminders).
Changes within the networks
Within healthcare networks complexity is increasing in two ways: an increase in the number of nodes (ie new stakeholders entering the network) and the changing nature of the ties between the nodes (ie existing stakeholders gaining more influence).
New stakeholders entering the network
There are new, significant stakeholders, entering the healthcare network and contributing to the increased network complexity. Examples are new governmental bodies and health authorities, new health insurers and new types of opinion leaders such as non-profit organisations.
For instance, new health authorities have been created to ensure patient safety, or quality and cost-effectiveness of therapy and care. Examples are National Institute for Clinical Excellence in the UK and more recently, IQWiG in Germany. These independent centralised organisations appraise new technologies and provide guidance on prescription and reimbursement decisions.
Major changes are also under way on the health insurance side. Despite the fact that private health insurance in most European countries is still purchased on a voluntary basis, private insurers are gaining significant ground. They play an important complementary, substitutive or supplementary role in healthcare financing, influencing the entire network.
Another major trend, contributing to new emerging stakeholders, is the uptake of more a holistic view of health and disease. Today, biological, mental as well as social factors are all accounted for in the prevention and therapy of pathologies. As a consequence, physicians are working more closely not only with physiotherapists, psychologists and social workers but also increasingly with professionals involved in alternative medicine such as acupuncture and homeopathy.
A growing amount of influential non- profit organisations are also emerging. Through new forms of media, they are reaching an increasing number of the stakeholders and actively shaping the opinion of the customers. Examples of such organisations are the European society for quality in healthcare (ESQH) and the Health On the Net Foundation (HON).
Existing stakeholders are gaining influence
Not only are new stakeholders entering the scene, but pre-existing stakeholders are increasing their influence on the prescription process and altering their roles in healthcare networks. Some of the evolutions are listed below.
- Governmental and formulary committees: Governmental bodies and formulary committees have become increasingly influential in the prescribing process.They have a direct impact through dictating lists or formularies of drugs to be prescribed for a certain condition, deciding which products will be reimbursed and at what condition, controlling the allocation of budget to certain disease areas and treatment options and promoting the substitution of certain prescribed drugs with corresponding generic drugs.(7)
- Pharmacists: As a result of legislative changes in some European countries, pharmacists are now, under certain conditions, encouraged to substitute prescribed drugs for corresponding generics, in order to achieve cost–savings. They are therefore becoming influential in the drug choice and control process, to the extent that in some countries, such as the UK, they are acquiring a limited prescribing role.
- Hospital managers: The general setting for the management of many European hospitals has undergone substantial changes during the last five to ten years, especially with respect to economic, personnel and technical resources.(8) Because of the modern hospital’s structural complexity, the increasing degree of specialisation among its work force, and an operating environment defined by rapid change, the classic hospital organisational culture has clearly been affected.As a result, several changes in power positions have occurred, in particular as hospital managers increase the scope of their decision making to healthcare provision.
- Patients and patient advocacy groups: Patient behaviour has undergone significant changes largely due to the emergence of Internet technology.They are becoming better informed, more empowered and, as a result, have increased their expectations of the healthcare industry.They demand a better service and want to have an increased influence on their treatment, thereby placing more pressure on the physician In addition, patients are becoming more organised through patient advocacy groups, such as the International Alliance of Patient Organisations (IAPO). Such advocacy groups and organisations have been successful in promoting patient-centred healthcare, increasing patient medical knowledge and allowing patients’ voices to be heard.
Implications for the pharmaceutical industry
Commercial success relies on a company’s ability to understand and meet customer needs. In a simple system where one stakeholder group, namely prescribers, fairly autonomously decides how to treat a patient, it is justified to focus marketing and sales efforts on that specific group. However, as demonstrated above, prescription power is shifting away from the physician as new stakeholders appear in the network and existing stakeholders increase their influence. Despite a physician being entirely convinced of the superiority of a product, his opinion will be of limited value if it that product is not on the closed formulary, if online patient forums are not favourable to the product, or if pharmacists are systematically substituting it. Such dynamics are facing the pharmaceutical industry with a fundamental change: the network is becoming the customer.
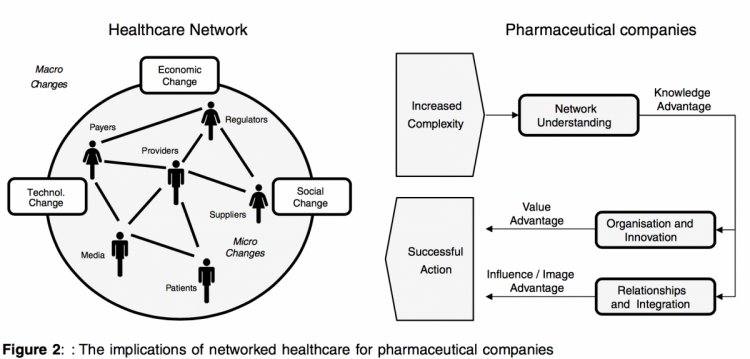
There is increasing evidence that pharmaceutical companies, who develop new capabilities and adapt their marketing and sales approaches to target the customer network as a whole, create an advantage compared to competitors who continue to drive the ‘share of voice’ model with physicians.There are three main advantages areas that ‘early movers’ can develop: (1) knowledge, (2) value and (3) influence and image (see Figure 2).
- Companies that view and analyse the customer environment from a network perspective and engage in more collaborative practices with the network stakeholders will quickly improve their understanding and knowledge of the needs and interests of the stakeholders and the network dynamics. This network understanding is a prerequisite for improving innovation, organisational alignment and relationship building with critical stakeholders.
- Companies can improve innovation and create more value for target customers and critical stakeholder by reorganising their sales and marketing operations to address the networked reality. For instance, companies can realign their formal structure to ‘mirror’ stakeholder segments in the healthcare network. In addition, companies can enable the systematic development of cross- functional competencies and services that dynamically address the changing needs of critical network stakeholders.
- Companies can positively influence image, trust and sales success by developing relationships and successful interventions with new influencing stakeholders.The long-term goal is to integrate the network, performing new roles such as ‘knowledge brokers’ and ‘network facilitators’, creating tailored service offerings that allow target stakeholders to operate more successfully in the networked environment.The implication is that pharmaceutical companies are not only reacting to changes in their environment but increasingly start to take a pro-active and legitimate role in shaping the environment together with other stakeholders.
Conclusion and outlook
This paper sets the scene, by defining the concept of networked healthcare, demonstrating how the healthcare industry is changing and outlining what the implications for pharmaceutical companies are. In particular, the last section highlighted why it makes sense for pharmaceutical companies to develop new capabilities and adapt their marketing and sales approaches to reflect the increasingly networked environment. However, the question of how this could be done still remains open. In the following editions of the Journal of Medical Marketing, three articles will provide in-depth ideas and examples of what can be done in practice by the pharmaceutical sales and marketing function to successfully operate in the increasingly networked reality.
Article 1 – Understanding networked healthcare: What concrete steps can pharmaceutical sales and marketing take to better define, map and ultimately understand the different stakeholders in the networked environment, including their influencing power and relations with each other?
Article 2 – Organising for networked healthcare: What organisational challenges do pharmaceutical companies currently face due to the increasingly networked environment and what concrete organisational changes could be made to address these challenges?
Article 3 – Integrating networked healthcare: How can pharmaceutical companies become more successful in their interactions with the various stakeholders and what type of activities allow these companies to change their role in the network?




