Five Steps to Find your ‘Beyond the Pill’ Strategy
Outcomes data are the holy grail of drug development and market access.

Everyone involved in healthcare – physicians, patients, governments and in particular payers – wants to see incontestable proof that the introduction of a new drug will result in meaningful and tangible ‘outcomes’. Of course, that is entirely reasonable and not new – clinical trial results have been the cornerstone of drug approvals for decades – but the nature, volume and level of scrutiny of outcome measures for reimbursement has changed and intensified in an environment where there are many more ‘me too’ drugs and a significantly more complex market access environment.
Clinical drug development rates have fallen. In the US, a 2014 study revealed that the success rate for bringing new medicines to market is nearly one in 10 – which is about half the previous rate.(1) A similar trend in approvals may be occurring in Europe - and that is before we even get to reimbursement. New drugs now need to demonstrate improvement over existing “gold standard” therapies that can vary significantly from country to country for various reasons, such as cost containment.
Many countries in Europe have set-up formal institutions to perform cost- benefit assessments, the most famous being NICE in the UK, established in 1999, and IQWiG in Germany, established in 2004 and still focusing particularly on incremental benefits despite the most recent legislative changes in 2011. While these have served their purpose well, they can represent a formidable barrier to national reimbursement, due to the very exacting level of evidence required against existing therapies.
It is in this context that the opportunities presented by a ‘beyond the pill’ strategy become apparent. Unless a new product is first-in-class or significantly differentiated in some way, pharmaceutical companies can no longer rely on the product alone to demonstrate its own value for reimbursement. Rather, the product must now form one part of a compelling package of services which are proven to make a positive impact on healthcare systems – in other words, it is the services created to support and complement a new drug that can now provide the ‘holy grail’ of outcomes data required for reimbursement. Many within pharmaceutical organizations have a vital role to play to make this happen – not least the in-house medics / physicians, who must assist in the design, verification and communication of many of the services and tools so central to this strategy.
But how should we go about choosing a “beyond the pill” strategy?
1) Start with the pill
We are talking about going beyond the pill but that does not depreciate the fundamental value of the therapy itself. The core product will always remain the most important factor, and you should start with the pill when thinking about how to go beyond it into mutually beneficial service provision.
The first consideration must be where your drug fits within the current therapy environment to understand the potential of the drug to compete on outcomes and/or have a unique selling proposition against competitive products.
This assessment should encompass
1) the nature of the disease – for example, any existing challenges around diagnosis of the condition
2) stakeholder needs along the patient journey - for example, the role of parents / carers for pediatric indications
3) the competition, such as competitive pharmaceutical brands or devices and
4) any specific requirements for the brand itself – e.g. IV infusions or first dose observations.
This initial drug assessment can start to lead you towards the kind of beyond the pill strategy you will likely need. For example, does your drug have superior clinical outcomes for specific patient populations? In that case, a conscious selection of services addressing specific steps in the patient journey is probably sufficient. Is your drug used to treat a complex chronic disease? Then you probably will need a platform for a wide range of solutions and services to improve outcomes. On the other hand, if your drug has very little differentiation on clinical outcomes, or is reaching the end of its life cycle, then you can employ beyond the pill services to increase loyalty with your stakeholders and maintain a premium over alternatives.
One thing is for sure - if your product is not significantly differentiated or will lose its unique selling proposition due to competitive brands to be launched in the near future, then there are compelling reasons to act. Drugs that are not differentiated on outcomes nor offer a unique selling proposition will likely see prices erode to generics levels due to pressures from healthcare payers. Reference pricing systems, such as the one in Germany, allow for a common reimbursement level or reference price for a group of medicines if they are considered “interchangeable.”(2) In effect, reference pricing allows payers to impose generic prices on drugs still under patent protection. Pfizer learned exactly that in Germany in 2005 with Lipitor, and Lipitor’s share of the German market subsequently collapsed by 75%.(2)
2) Find a Service Model Archetype
After considering where service opportunities will broadly fit with you product and likely resonate with your target customers, a decision on the service model archetype is necessary (see image). For each brand a decision needs to be made based on two key factors - firstly the optimal breadth of the services offered and secondly the level of customization.
Given the high cost of services and threat of margin dilution, a limited offering in line with stakeholder expectations can be a safe choice, particularly if sufficient to achieve a competitive advantage for a company’s drug, such as companion diagnostics for patient stratification, for example KRAS mutations for colorectal cancer or non- small lung cancer. Despite being a ‘limited’ offering, the outcome improvements can be significant due to the improved efficacy of focusing on responders (and excluding non- responders).
Highly customized services targeting one or few steps in the patient pathway represent a focused offering, such as patient monitoring demonstrating treatment success, e.g. complete and major molecular response based on BCR-ABL transcripts for patients with chronic myelogenous leukemia (CML). Good monitoring represents a very effective use of healthcare funds, particularly if novel generation drugs can lead to permanent cure, eliminating life-long chronic treatment costs altogether.
A broad offering can bundle generic services targeting most steps of the patient pathway to maintain high profile - a prerequisite for success of blockbuster drugs. For example, comprehensive patient compliance tools for payers and patients have been offered for oral bisphosphonate osteoporosis drugs before the availability of quarterly or annual infusions. Yearly expenditures for the consequences of patient non-adherence have been estimated to be hundreds of billions of US dollars, providing ample room for creating value from beyond the pill services.
Complete solutions that are highly customized and cover the entire patient pathway lead to relationship offerings for complex to manage diseases, often coming at a significant cost to build and therefore being amortized across a range of (high-price) biologics products, such as BioAdvance developed by Janssen to provide a comprehensive and very personalized approach to patients with various types of severe inflammatory disorders being treated by Remicade, Simponi or Stelara.
Developing economies can leverage personalized and scalable patient services relying on modern technology, such as smart phones, as the major alternative to traditional healthcare, thereby increasing access to a much larger part of the population while reducing overall healthcare costs significantly, opening-up opportunities to “own” a therapy area for drug companies.
3) Consider if “owning” a therapy area is a possibility
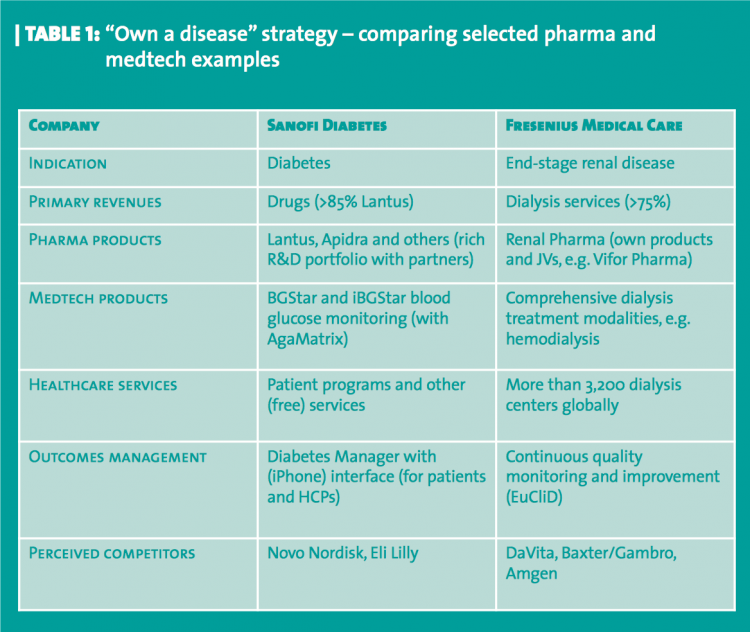
A complete solution strategy can enable pharmaceutical companies to potentially ‘own a disease’ through beyond the pill services. It is not an entirely new concept - Novo Nordisk, for example, ‘owns’ diabetes care from the pharmaceutical company perspective for many decades, with an impressive portfolio of pharmaceutical and complementary drug delivery devices supported by an extensive corporate program delivering high quality services to the diabetes community. Meanwhile one of its competitors in diabetes – Sanofi Aventis –contested the marketplace with assertive communications around its products, particularly its flagship insulin Lantus. Sanofi Aventis has since widened its remit to occupy similar ground to Novo Nordisk in terms of disease ownership, forming a dedicated diabetes business unit in 2010 to become a 360 degree solutions provider.
Very few pharmaceutical companies have started to integrate products and services holistically for a specific disease in the way that Novo Nordisk, Lilly and Sanofi Aventis have done for diabetes, but medtech companies – inherently more integrated into the workflows of their clients – have been able to push the envelope further than most. Fresenius Medical Care, for example, has now completed a transformation to a fully integrated dialysis services and products supplier.
The window of opportunity for healthcare products companies is still open in most diseases, despite an acceleration of the rapid growth of specialized healthcare service provider chains. It is important that companies take advantage of the window of opportunity soon.
4) Decide how far beyond the pill to go
‘Owning’ a therapy area through service provision is about as far beyond the pill as it is possible to go – and this obviously won’t be the right strategy for many situations. Deciding just how much to wrap around the product is a central consideration when determining a beyond the pill strategy.
Product-centric strategies have services at their core which address drug or device-specific issues along the patient journey that improve outcomes or increase the loyalty of stakeholders to that particular product. They are almost entirely reliant on drug (and/or device) revenue streams and usually demand a very apparent return on investment.
On the other hand, forward integration into services and solutions can open up novel revenue streams. Fresenius Medical Care, for example, has successfully implemented a variety of revenue mechanisms across countries, such as “razor-and-blades” pricing for dialysis equipment and consumables charged to centers, “fee-for-service” pricing per dialysis with payers, and long-term government contracts with negotiated quality and service levels and prices. Such business models may become the template for pharmaceutical companies in the future, particularly when a set of key success factors are met.
Companies should thoroughly map out a “holistic value chain” which delivers all steps of the services strategy – but it is important to note that stakeholders other than the pharmaceutical company itself – for example, home care services or medical call centers – will likely be best placed to implement some of the steps along the way. Independent of who provides the services, physicians working in drug development, regulatory affairs, medical affairs, drug safety or other departments will have an important role to play. They will have to extend their capabilities in observational research, safety monitoring, patient reported outcomes and other areas to cover all the aspects their pharmaceutical employers are ultimately responsible for along the healthcare value chain.
5) Act now, while a window of opportunity still exists
“Beyond the pill” is an umbrella term for a wide range of services from the simple, tactical necessities, to the all- encompassing strategy of ‘owning’ a disease. While the types of services differ enormously in scope and aim, one thing unites them all – they are here to stay.
In an ever-increasingly competitive and overcrowded marketplace, it is vital to have services in place which support your audiences in meaningful ways along the patient pathway and provide vital sources of differentiation for your products. Being able to generate superior outcomes through services is likely to have a positive impact on reimbursement and longevity of success, and ward off threats such as reference pricing systems.
Certainly, pharmaceutical companies will need to leverage healthcare services to demonstrate outcomes improvements in the real-world setting in the future, particularly for complex, chronic diseases with limited patient adherence, such as COPD and diabetes. Meanwhile, global medical device companies may currently be best positioned to exploit the strategic opportunity of integrating a variety of healthcare products and services to offer holistic healthcare solutions.
But it is important to act now – although “beyond the pill” is a reality already, many opportunities still exist within this space, particularly in terms of ownership of a disease area, or elements within it. Once these opportunities are snapped up, it is much harder to challenge within the same space. Of course, finding the right strategy is just one part of the battle – you then need to implement it, which involves a wide range of considerations, from who within your organization – including in-house medics / physicians – should be responsible for implementation, to which stakeholders and partners you need to involve along the way.[3] But with the right beyond the pill strategy in place, the holy grail of superior outcomes – for your stakeholders and your product alike – can be achieved.

References
- Hay M, Thomas D, Craighead J. Clinical development success rates for investigational drugs.
Nature Biotechnology 32, 40–51 (2014) doi:10.1038/nbt.2786 Published online 09 January 2014
http://www.nature.com/nbt/journal/v32/n1/full/nbt.2786.html - Dylst P, Vulto A, Simoens S. Reference pricing systems in Europe: characteristics and consequences.
Generics and Biosimilars Initiative Journal (GaBI Journal). 2012;1(3-4):127-31.
http://gabi-journal.net/reference-pricing-systems-in-europe-characteristics-and- consequences.html - Ruzicic A et al. Beyond the pill. Pharmaceutical Marketing Europe. November 2013, p. 26-28








