Going Beyond The Pill: The Big Questions

The challenges currently facing the pharmaceutical industry are numerous, well documented, and have led to a re- evaluation of the strategic approaches companies need to adopt in order to successfully commercialize their brands.
At the forefront of this re-evaluation is the concept of going ‘beyond the pill’ – in other words, offering services that address stakeholder needs along the patient pathway, leading to better health outcomes while at the same time providing a source of competitive advantage and higher value to patients, physicians and payers.
Pharmaceutical companies are beginning to accept the benefits of this approach and some are already starting to commit to this strategy. By focusing on the unmet needs of the stakeholders who regulate, reimburse, prescribe and take the medicines they produce, companies can provide targeted solutions which both help to contribute to better health outcomes, and create the optimal environment for their own products to thrive.
While the theoretical case for ‘beyond the pill’ is becoming well established, it is still a relatively new concept for the industry to actually put into practice. As a small group of passionate pharma employees continue to find their way in this area, we look at some of the main questions being raised as they try to come up with practical ways of getting there.
Q1) Is ‘Beyond the Pill’ the same as adherence?
When considering the types of benefits and services beyond the pill could potentially provide, improving adherence will always be near the top of the list. Adherence to medication has been an issue for as long as people have taken pills; the World Health Organization estimates that between 30 and 50% of medicines prescribed for long- term illness are not taken as directed, so it continues to be a huge unmet need.
Better adherence would benefit everyone – patients, payers and yes, the drug companies. But while this is certainly a big opportunity and a fundamental aspect of many beyond the pill initiatives, it is not the only one.
It is vital that patients are at the center of a beyond the pill strategy to make it meaningful in terms of outcomes, but there are several ways in which patients can benefit beyond an increased likelihood to take their medicine. Beyond the pill strategies can encompass several aspects such as disease and therapy awareness, diagnosis, initiation of therapy, improving access to medications and general patient support.
When the support is there and addresses a key gap in the patient pathway, the link to therapy is tangible for patients. A recent US survey revealed that 75% of online consumers who used pharma patient support programs said they feel confident the prescription they have is right for them, or for those they take care of, because of these services.
Some beyond the pill programmes will of course focus primarily on stakeholders other than patients, most commonly healthcare professionals such as nurses, or payers, but the overall strategy should keep the patient – but not necessarily just patient adherence – at the center.
Q2) Whose responsibility is it anyway?
Probably one of the most common questions companies have around ‘beyond the pill’ is where the planning and strategy should originate from within the organization.
While it doesn’t fit naturally into any one existing job categories, marketing may seem like the most natural fit as many of the types of services provided in ‘beyond the pill’ have traditionally been considered marketing-type activities.
A poll on the Beyond the Pill LinkedIn group posed this very question, with marketing receiving 30% of the vote, compared to 54% for the executive level, with the remainder shared between R&D, sales and other.
From the poll it is clear that committed leadership is a prerequisite for success, however, the functional lead probably lies elsewhere within the organization. Ultimately, who leads it is probably less important than establishing a cross- functional team that has the principal responsibility of owning and driving the beyond the pill programs.
Marketing and medical should certainly be represented within this team and legal / compliance input is essential. External partners may be required to ensure any gaps in knowledge are filled (for example on the latest service developments, logistical and technical requirements, and cross- country implementation support).
Q3) How do we know which services to provide?
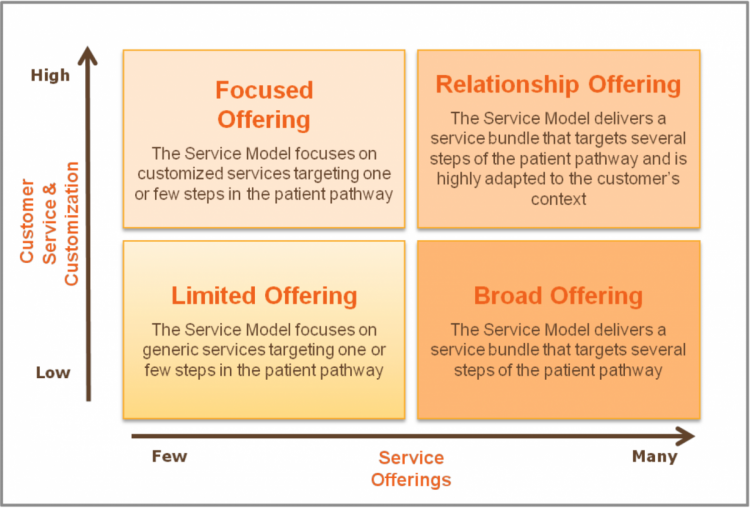
A beyond the pill approach should have a central strategy at its core which underpins all services offered. The service strategy should include in-depth customer analysis as well as disease, brand and competition mapping, resulting in a detailed assessment of stakeholder needs throughout the patient pathway. The completed mapping forms the basis from which the service model strategy can be developed, involving prioritization of the service model components and development of the proposed solutions.
An example approach to this mapping process is the service model archetype (see image), which allocates certain service approaches based on the types of factors listed above. This can support decision- making in terms of the breadth and depth of your beyond-the-pill strategy.
Q4) What is the return on investment of the beyond the pill approach?
Measuring return on investment with provision of services can be notoriously difficult. Yet the question will be asked again and again, until their financial value is proven.
There are certainly quantifiable outcomes for many services beyond the pill, whether its numbers of patients entering a support program or completing a course of treatment, or number of app downloads by healthcare professionals. There are also outcomes which are much more difficult to measure, for example the added confidence of doctors, payers and patients in a brand or company, but they are none the less important for that. Some of these can be translated into ROI, many cannot.
Either way, the beyond the pill concept is changing from something ‘nice to have’ to something essential, which will likely become an everyday part of expected pharma industry provision. Therefore it is likely that measurement will become more and more tangible and more directly linked with improvement of health outcome, which would justify the sale of the product.
Indeed Joseph Jimenez, CEO at Novartis, recently stated his belief that pharma companies in the future “are going to be paid on patient outcomes” rather than on just selling prescription drugs. This idea is gaining some traction, and it is almost certain that measuring patient outcomes will become more and more central to reimbursement.
Published on: http://social.eyeforpharma.com



