Market Access for Specialty Products in Latin America
Andrea Sobrio and Dr. Sandra Schoenes examine the market access challenges and opportunities specifically for premium, specialty inpatient products in the LatAm region.

The pharmaceuticals market in the Latin America (LatAm) region is experiencing a period of healthy growth. It is estimated that the region’s eight major countries — Brazil, Mexico, Argentina, Chile, Colombia, Cuba, Peru and Venezuela — represented a market retail value of $80bn in 2013, up from $50bn in 2010. Opportunities exist both within the public and private sectors, but the biggest potential is arguably with private payers — in particular, premium specialty products can provide good returns with the right, tailored approach. But market access environments vary widely across LatAm, and there are specific access challenges for premium products.
A heterogeneous region
There is no ‘one size fits all’ approach to market access in Latin America — while it is an attractive region overall for pharma, each country is unique and companies must tailor their approach and be sensitive to national variations.
There are significant differences in pricing and reimbursement across the region. Some countries, such as the region heavyweight Brazil, utilize HTA assessment for pricing, while others such as Mexico use reference prices; others (e.g. Chile and Argentina) leave it to the companies to decide price. However, the landscape is dynamic and needs monitoring, with Colombia as one example transitioning from free pricing to reference pricing.
In terms of reimbursement, there is a wide range of payers — from health plans and insurers, to hospital financial management and health department officials — all trying to find a balance between the need for cost- containment and increased consumer expectations for improved healthcare.
Clustering the LATAM countries to make strategic decisions
To bring their premium products to these markets, pharmaceutical companies need to ensure there is tight alignment between global HQ and local operations. It is important that markets are clustered effectively to sequence and prepare launches — this is something that local operations can also benefit from, sharing learnings across markets within the same cluster.
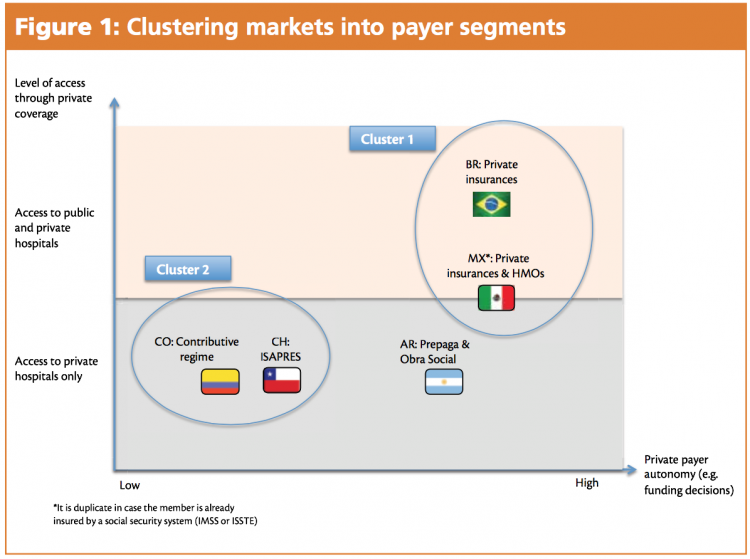
Figure 1 shows one way of clustering markets into private payer segments, based firstly on their degree of autonomy (e.g. the degree to which funding decisions can be made without influence by national or regional health authorities) and secondly on the level of access through private coverage (e.g. if members of the private sector also have access to a public health sector).
Understanding just how quickly and through how many stakeholders (e.g. including national and regional health authorities) listing decisions are made is vital, and dictates where the country is on the degree of autonomy x-axis in the Figure 1 graph. In countries with high levels of private payer autonomy — e.g. Brazil and Mexico circled here in cluster 1 — private payers are free to decide which drugs they reimburse in any of the multiple health plans they offer.
In countries with a low level of private payer autonomy — e.g. Colombia and Chile in cluster 2 — the private payers have a reduced level of freedom regarding funding decisions. In Colombia for example, the contributive EPS — the HMO segment, which subcontracts mostly to private providers — needs to reimburse all drugs on the national health formulary (POS). At the moment this national formulary does not include most premium drugs, but with the upcoming healthcare reform, this could change.
The level of access of those with private coverage (the y axis on the graph) is also an important consideration. Firstly, access to both public and private hospitals gives physicians in public institutions access to, and experience with, patients taking premium, innovative medicines. Secondly it usually means that the private sector has more freedom in making coverage decisions as the citizen is already covered by a national health insurance.
Mexico and Colombia — two divergent opportunities
Countries representative of the two clusters we have highlighted include Mexico — the second largest LatAm market behind Brazil — in cluster 1, and Colombia — a complex market due to its dependence of national funding policies — in cluster 2.
Mexico
The private sector in Mexico has a limited patient base — only 3.5% of population — but provides a relevant benchmark in terms of early product adoption and purchasing power.
Private payers can be divided into two segments — “normal” private insurances and HMOs. Unlike “normal” private insurances, HMOs have non- mandatory formularies, where selected premium drugs (over $10,000) can be included. However, since 2012, all private and HMO insurances carry one-time and usually non-renewable policy limits.
Depending on the policy these limits can be prohibitive for the use of premium innovative drugs.
In addition, there is a smaller segment of patients seen in private hospitals who are very wealthy individuals (often “health tourists”) who pay “out-of-pocket” for products prescribed by their treating physician.
On the public sector side, most premium innovative drugs are classified as “clave 5000” and their prescription is rare outside certain specialist hospitals. The few granted access now have to face extra layers of approval before reaching the hands of doctors — the two major public payers (IMSS and ISSTE), have both recently introduced a new prescription control program (called Catálogo II at IMSS), which restricts and delays access to premium innovative drugs by up to three weeks due to a centralized pre-authorization and drug delivery process.
Colombia
Colombia currently has near-universal coverage, something rarely seen in Latin America. The financial strain however, has created the need for change, and the country is entering a period of transformation.
Currently, Colombia’s health system operates under two schemes; contributory and subsidized. Forty percent of the Colombian population holds formal employment and receives health insurance through the contributory scheme, granting access to private hospitals. The remaining 60% of the population are subsidized by the public health system.
The greatest potential for premium in-patient drugs lies within the contributive EPS. This is because the use of premium drugs is higher in private than in public hospitals due to their increased purchasing power, their strong negotiation power, and the existence of independent funding, if the hospital has the status of a foundation with independent resources.
The contributive market is currently fragmented into 21 players (some of them also offering subsidized insurances). A key factor differentiating Colombia from other Latin American markets is this de-centralization of key customers over the country. Being successful in Colombia means being able to adapt to this structural and geographical reality.
Premium innovative drugs are usually excluded from the national compulsory health plan (POS). In order to prescribe a non-POS drug, the hospital needs to send a request to the EPS in charge of the patient — this is either authorized and reimbursed, or rejected. Although the cost for the drug is not borne by the EPS, they have incentives not to approve non-POS treatments.
However, two major changes proposed in the healthcare reforms are imminent — firstly the abolition of funding for non-listed treatments, and secondly the creation of a unique national fund for direct hospital financing. The implementation of a unique benefit package (Mi Plan) is expected to represent an additional market access hurdle.
Overcoming the hurdles and achieving access for premium, specialty products in LatAm
There are two overall potential strategic approaches to market access in Latin America — independent development or partnership. The decision on which to implement will depend largely on a) the current company presence within the target country, and b) the level of company experience with in-patient products.
Those without any existing country presence should develop a LatAm market access strategy and then aim to set up an appropriate “critical mass” organization. This can either be achieved by mergers and acquisitions or by partnership with a local distributer or non- competing manufacturer. Alternatively, the company can decide to invest significant resources in building-up an organization with the required capabilities in the target market(s) systematically over the medium-term. Those with a presence in the target market but limited in-patient product experience will essentially need expert consultation to guide them through.
In countries where low private payer autonomy exists, a dual public-private approach should be taken, in order to achieve national product endorsement (e.g. national listing, inclusion into national clinical guidelines) while achieving private payer coverage.
In countries where private payers have a high level of autonomy, the manufacturer can focus on the private sector and market access is generally quicker. It is also worth targeting leading public reference centers, given their influence on private hospitals.
In the long term, pharma companies can shape and develop their markets by aligning with payers to create novel insurance options, particularly if they possess a rich portfolio of high-cost products in a yet underfunded therapeutic area.
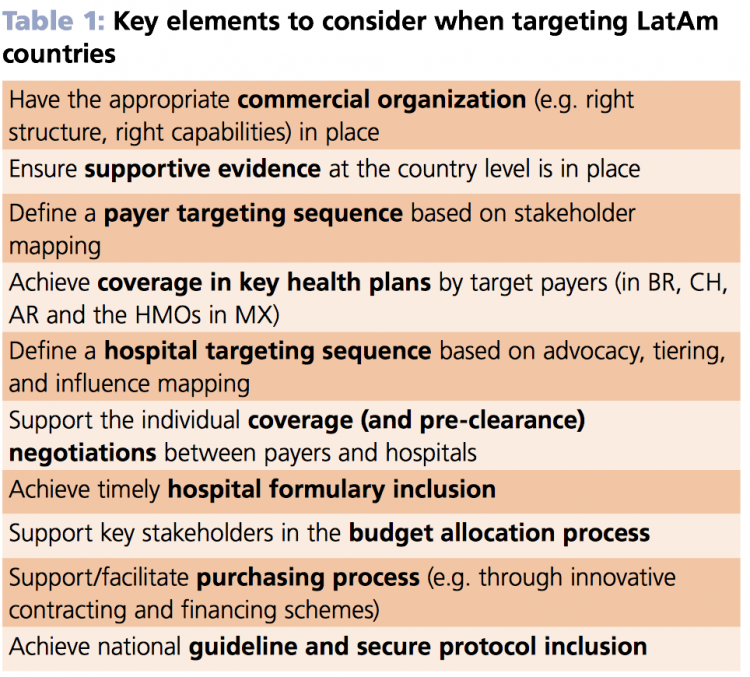
Several other essential factors should be considered in each case (see Table 1). But what specific steps could be taken to facilitate hospital access in the two example markets we have highlighted?
Access to Mexico
To achieve hospital access in Mexico, try to facilitate the use of your product in reference institutions, which can be both private and public (e.g. tertiary care IMSS hospitals). Doctors who use the product and work across both settings can be powerful advocates.
You can also consider organizing medical education programs in partnership with the reference institutions, and establish preceptorship programs for other doctors to visit reference hospitals.
However, it is important that key account managers are in place on the ground to liaise with individual physicians about the benefits of the product, as protocols are only loosely followed in private hospitals.
Access to Colombia
In Colombia, a discount pricing agreement may be essential to incentivize the hospital to include your product in the formulary, and this may include portfolio agreements and Managed Entry Agreements.
In the case of an acute care drug, it is advisable to avoid pre-clearance and instead facilitate approval post-use by facilitating supportive clinical and health economical evidence for your product and implementing medical education of prescribers to ensure correct and rapid patient identification.
To help achieve formulary inclusion you should build KOL and medical society endorsement and consider investing in local cost- effectiveness and cost-benefit studies.
Make sure you map the budgeting process in the different hospitals in order to identify the key stakeholders, and then support them with a budget forecast tool as well as with a business case for your product.
Conclusions
The LatAm region holds significant potential for pharma, but achieving market access for premium specialty products requires a customized strategy accounting for the high level of heterogeneity of the countries.
Clustering markets by level of private payer autonomy and by level of access to public and private hospitals provides a starting point for an effective market access strategy.
It is critical to perform a market access assessment at country level in the pre-launch phase to develop country launch roadmaps and inform the launch sequencing.




