Innovative Contracting: A Review
Executive Insight has conducted in-depth research into recent innovative contracts implemented across Europe to assess their benefits and limitations, and learnings for the future. This study incorporated a comprehensive literature review and key stakeholder interviews in EU big 5 countries, including pharmaceutical companies, payers, healthcare consultants and governmental bodies, across several major therapy areas. This is a summary of the key findings.

Selling in a time of cost containment
Despite the current challenging economic climate, spending on healthcare continues to increase. Life expectancy continues to rise, along with incidence of chronic diseases like diabetes and cardiovascular disease. Modern day public expectations of a higher quality of life also increase the demand for high quality health-related services and products. At the same time there are stricter clinical targets and expensive new product and health technology launches. The net result is a rise in the overall cost of healthcare provision.
Policymakers recognise that the pharmaceutical industry is a major factor in on-going rises in healthcare expenditure. In the OECD (Organisation for Economic Co-operation and Development) countries, pharmaceutical spending accounts for 17% of total health spending and 1.5% of GDP on average (Nason and Sproule, 2011). Although pharmaceutical growth has slowed since the 1990s, growth in pharmaceutical expenditure continues to exceed the average growth of OECD economies (Nason and Sproule, 2011).
As the amount of health care demanded is starting to exceed the available resources, EU countries are now faced with common problems in delivering equal, efficient and high quality health care services at affordable costs.
In response, governments and policymakers of EU member states have often focused on employing new strategies, such as cost-control measurements, to meet the challenges in health care delivery and to stem the growth in health spending. These differ from country to country, but commonly included the implementation of co-payments; regulatory policies to cap profits; standardised prices using global reference pricing and international comparisons of medicines; and the introduction, and use, of health technology assessment (HTA) as well as cost-effectiveness analysis (Sotiropoulos, 2011).
The assessment of a new drug is no longer based on the traditional regulatory hurdles of quality, safety and efficacy alone. Payers and regulators want reassurance on the benefits – both human and economic – that a drug will bring post-approval and launch. This information usually relates to clinical benefit, i.e. short-and long-term effectiveness as well as safety or possible interactions with other therapies; or value for money as well as the economic impact or overall cost to the payer (Hunter et al, 2010). There is tremendous pressure on approval and reimbursement decisions now, and the key for payers is minimisation of risk.
So in this challenging climate, how can a pharmaceutical company convince payers and regulators that its new treatment is worth finding the budget for? And in particular if other therapeutic alternatives are available?
Innovative Contracts
We have observed many companies shifting the weight of their resources to payers and key accounts, with increased investment in pricing strategy, payer collaborations and health economics. But even with more resource and improved dialogue established, it is still vital in the current environment to identify compelling ‘win-win’ scenarios with risk minimized for the payer.
This is where innovative contracts come in. Innovative contracts between manufacturers and insurers originated in the US in the 1990s (Sotiropoulos, 2011). These schemes were ‘no cure, no pay’ strategies for baldness drugs, schizophrenia and cholesterol-lowering statins and had only little success. Money- back guarantee schemes followed in the UK in 2000, which were more successful. These outcome-based schemes in the UK were concluded following recommendations made by NICE not to cover drugs based on lack of cost-effectiveness.
Nowadays, various innovative contracting models are in use in many countries, such as the UK, Australia, Canada, Italy, Germany, France, Sweden and Spain. Different countries apply different forms of innovative contracting models and mechanisms, and use different terminologies. Some countries consider these contracts as another tool for controlling expenditure on drugs, while other countries apply more substantive arrangements, dealing with outcomes research, information, or compliance for example.
For the purposes of this paper, an innovative contract is defined as an ‘agreement concluded between pharmaceutical companies and payers implemented to relieve the impact on the payer’s budget of innovative medicines brought about by either the uncertainty of the health benefit or value of the medicine and/or the need to work within finite budgets.’ (Adamski et al, 2011). In other words, it helps to minimise risk for payers, which in turn helps to secure market access for pharmaceutical companies, while often having the added benefit of producing additional ‘real world’ data.
While the concept of innovative contracting is theoretically beneficial for payers and pharma companies alike, do they work in practice?
Executive Insight has conducted in-depth research into over 60 recent innovative contracts implemented across Europe to assess their benefits and limitations, and learnings for the future. This study incorporated a comprehensive literature search, review and appraisal of peer-reviewed and other literature in Germany, the UK, Sweden, Italy and France, and 22 key stakeholder interviews in EU big 5 countries, including pharmaceutical companies, payers, healthcare consultants and governmental bodies, across several major therapy areas.
Methodology
Literature review
A comprehensive literature search, review and appraisal of both peer-reviewed and non-peer review literature as of 2008 were performed to obtain a comprehensive overview of existing academic literature on the issue.
The focus was on European countries, primarily the UK, Germany, Italy, France and Sweden, because these were the countries with the largest pharmaceutical market and/or which were known to apply such strategies.
For the final analysis, 34 papers were retrieved for full review, including peer-reviewed and non-peer reviewed literature. These papers were evaluated for relevance, and their reference sections were analysed for other potential references.
Stakeholder interviews
In addition to the existing literature and documentation on this topic, key stakeholders were interviewed to obtain a comprehensive overview of the types of innovative contracting models in use.
The key stakeholders included pharmaceutical companies, payers, lawyers, healthcare consultants, doctors, governmental bodies, physician organisations and University professionals. In total, 22 key stakeholders from Germany and the UK were interviewed.
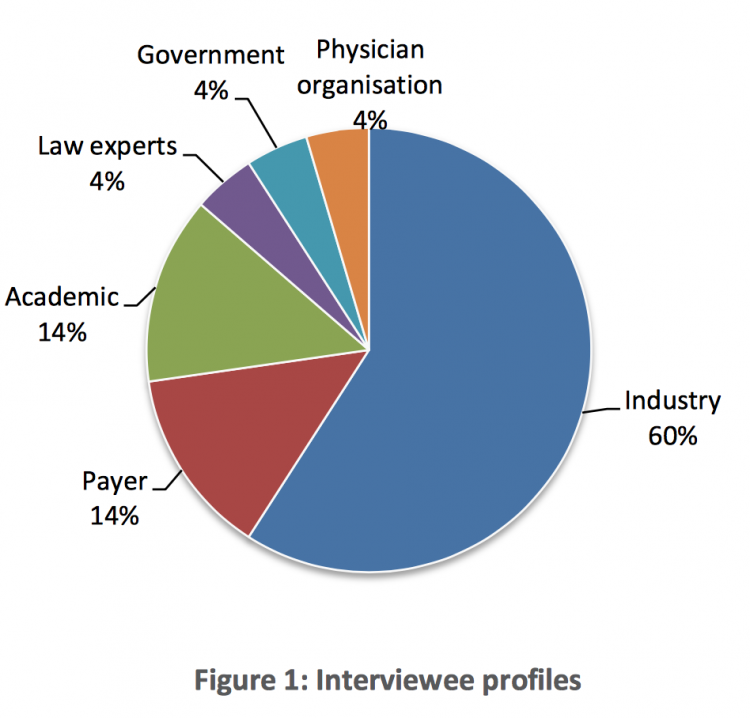
The questionnaire used for the interview included 27 questions in total divided into three different parts: what type of innovative contracting models are currently applied between pharmaceutical companies and payers; the experiences made with these contracts and what type of contracts are being favoured by which stakeholder.
Finally, based on the findings from the literature review and the stakeholder interviews, a framework was created, with the aim of assisting stakeholders in the decision making of an innovative contract.
Types of Innovative Contract
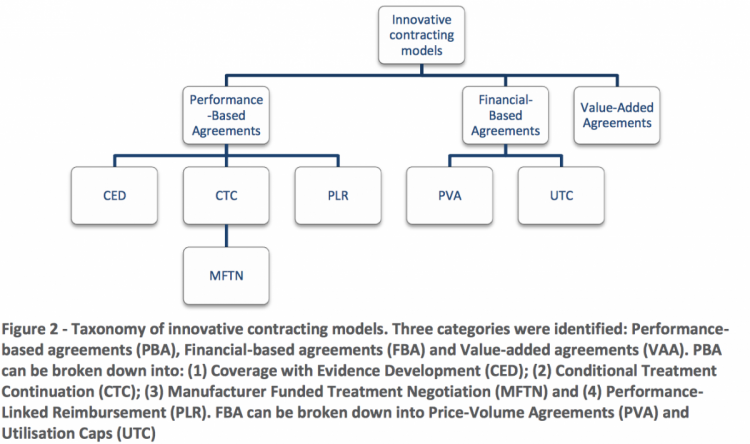
Based on our research we have identified seven types of contracts which are commonly utilised, which can be broadly split into three main types of agreement: Performance-Based Agreements (PBAs), which provide specific performance-related conditions for reimbursement for treatments, Financially-Based Agreements (FBA) which generally focus on controlling the total commitment of expenditure by the payer and Value-Added Agreements (VAA) where manufacturers offer discounts but also provide the patients with additional services to ensure optimal medical treatment.
Figure 2 outlines how the seven types of innovative contract fall under these three main categories. Financially-Based Agreements include Price-Volume Agreements (PVA) and Utilisation Caps. These are often also referred to as market share agreements, cost-sharing agreements and price caps. Performance-Based Agreements can be broken down into Coverage with Evidence Development (CED) schemes, Conditional Treatment Continuation (CTC) schemes, Manufacturer Funded Treatment Negotiation (MFTN) schemes and Performance-linked Reimbursement (PLR) schemes. The third standalone category contains the Value-added Agreements (VAA).
Coverage with Evidence Development (CED)
These schemes are designed to address flaws in the existing evidence base for the drug. The scheme allows for reimbursement of a product at a price set by the manufacturer, for a pre-determined period of time. After this period, a binary coverage decision is conditioned upon the collection of additional evidence from the population in order to support continued, expanded, or withdrawal of coverage (Carlson et al, 2010). If the product has failed to show any value, the payer withdraws the price and sets it lower against existing standard of treatment. There are two ways of how CED schemes may be implemented: (1) Only in research, where only patients participating in a scientific study are covered; (2) Only with research, in which all patients are covered conditional on a scheme to conduct a study that informs the use of a drug in the full patient population (Carlson et al, 2010).
Conditional Treatment Continuation (CTC)
Under a CTC scheme, the continuation of coverage for individual patients is conditional upon meeting short-term treatment goals (surrogate endpoints or biomarkers). Treatment is only continued if a positive response is observed in the patient. In most schemes the manufacturer provided discounts during the treatment initiation period (Carlson et al, 2010). Once a positive response can be observed, the payer continues to cover these patients. Manufacturer Funded Treatment Negotiation (MFTN) In some CTC schemes, the manufacturer pays the full cost of initial treatment, until enough evidence is provided to convince the payer, who then continue to cover the treatment for responders. These schemes are referred to as MFTN (Carlson et al, 2010). The schemes are implemented mainly due to the payer’s concerns that patients are receiving continued treatment despite a lack of health benefit.
Performance-linked Reimbursement (PLR)
PLRs aim to relocate financial incentives to guarantee rewards for therapeutic efforts that produce high quality care. Under these schemes the manufacturer provides rebates, refunds or price adjustments if their product fails to meet an agreed upon outcome (health improvement). The outcome can be an improvement of short-term clinical data, measured in surrogate endpoints or biomarkers; long-term clinical data, measured in primary endpoints; or adherence to treatment. Such schemes have been mainly used when evidence for the health gain from the drug is insufficiently robust from the payer’s perspective, whereby the manufacturer is sufficiently confident in their product such that they are prepared to accept a lower reimbursement price if it does not achieve the desired outcome (Carlson et al, 2010).
Price-Volume Agreements (PVA)
These schemes focus on controlling financial expenditure and/or enhancing the value proposition of the new drug. PVAs, also called cost-sharing or budget impact schemes, work on a population level. In most schemes, a new drug’s reimbursement price is linked to a sales volume threshold. The manufacturer must provide compensation, in form of price reduction or cash payments to the payer, if a pre-agreed drug sales threshold is exceeded (Adamski et al, 2011). Utilisation Caps These schemes are similar to PVAs, but are at the patient level. Under these schemes, utilisation by patients is measured. In most of the schemes, a threshold of drug dose or treatment cycles is set, up to which the payer covers the drug. Once this utilisation threshold is exceeded the manufacturer pays for further treatment (Carlson et al, 2010).
Value-added agreements (VAA)
Under these schemes, manufacturers offer discounts but also provide the patients with additional services to ensure optimal medical treatment (Hogan and Hartson, 2008). These services may be support programs, educational programs, general practitioner training, homecare visits by qualified nurses, to name a few.
Geographical distribution
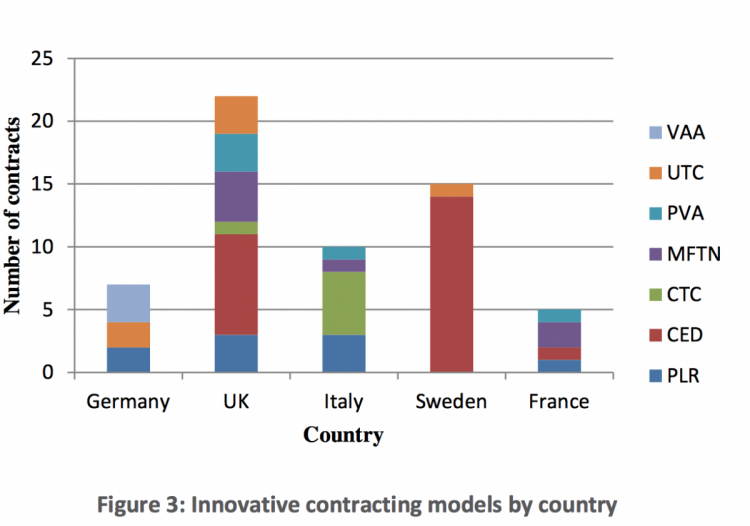
The geographical distribution is shown in figure 3. Most contracts were concluded in the UK, followed by Sweden and Italy. The UK and Sweden used to the largest extent CED schemes. The UK applied all scheme types except VAAs. VAAs were only applied in Germany. Italy mainly used the CTC schemes. All countries used PLR schemes except Sweden. CED schemes were used most frequently followed by PLR.
Therapeutic areas
Innovative contracts are mostly used for drugs that relate to high cost or high performance. Figure 4 shows the conditions for which most innovative contracts were applied – oncology was the therapeutic area associated with most innovative contracts by some margin.
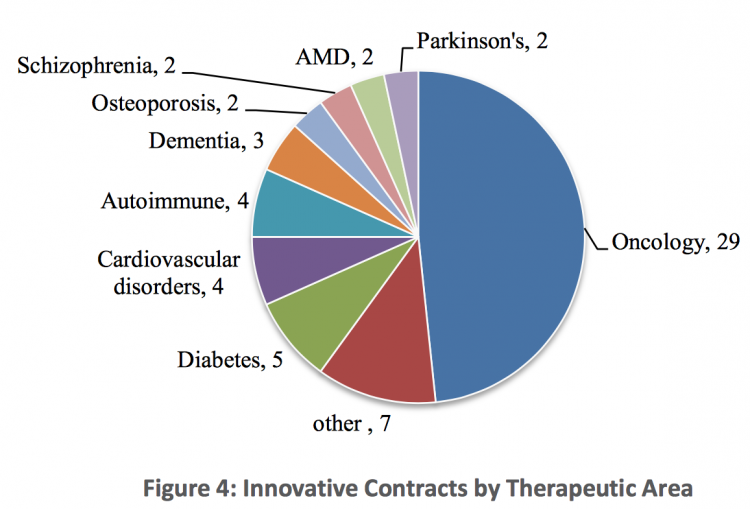
A distribution of which contracting form is used for which disease area is shown in figure 5. Except for VAAs all contracting types were applied to oncology medicines. CED schemes were applied to nearly all therapeutic areas except dementia, osteoporosis and AMD. CTC schemes have only been used for cancer drugs. For Parkinson and Schizophrenia only CED schemes were applied and for Osteoporosis, only PLR schemes were used.
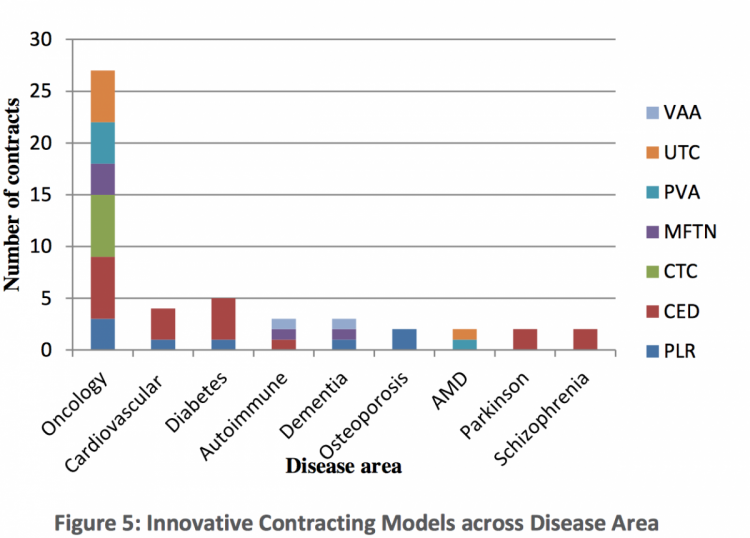
What are the benefits?
Our research showed that innovative contracts are associated with several benefits. They can help pharmaceutical companies from a financial perspective, achieving faster market access, higher sales volumes and faster patient access to drugs, but can also improve performance and outcomes (i.e. better patient care), and provide data demonstrating the cost-effectiveness as well as patient outcome in the real care setting (‘real world’ data), both of which are also important to payers. Most importantly from the payers perspective is the ‘safety net’ provided by these types of agreement, minimising any budget impact risk associated with committing to reimbursement for a new medicinal product.
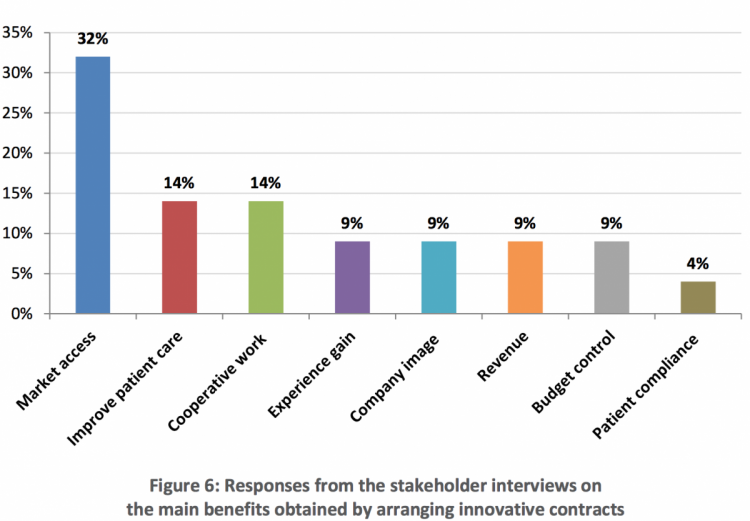
What are the issues?
While the potential benefits of innovative contracts are relatively straightforward, our research has unearthed several concerns.
The greatest concern, expressed by around half of the stakeholders we spoke to, is the high administrative burden, a problem that particularly seems to be associated with PBAs. For example, many schemes require significant additional patient monitoring and data collection to verify whether the stipulated conditions have been met. This administrative burden and the associated extra cost are the reasons why most stakeholders prefer using rebate schemes or simple FBAs.
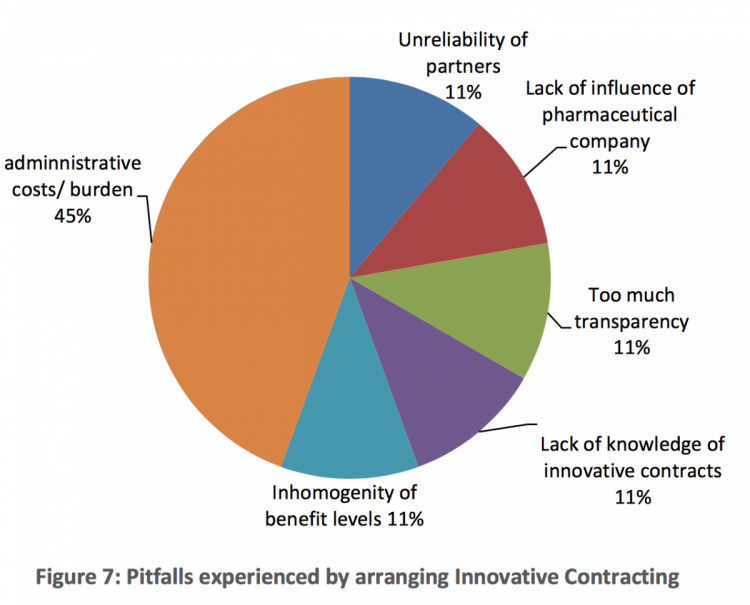
Another difficulty that can arise is agreeing on a surrogate endpoint or biomarker, whereby a drug can be judged as having worked or not.
Stakeholders also state concerns about a lack of trust that exists between pharmaceutical companies and payers, which may restrict collaboration and make negotiations difficult.
A lack of inclusion and transparency for doctors and their patients is also a perceived problem. Many doctors criticise the lack of transparency of these contracts, stating that patients and providers are not given enough information on the structure and benefits.
Several concerns with devising innovative contracting were identified from the literature. In most cases, the failure of a scheme was not necessarily due to an inadequacy of the drug itself but a ‘malfunction’ in the design of the innovative contract.
Lessons for the future
Among the most commonly mentioned critical success factors was that the product itself is paramount – a quality drug with a high value will always fare better, and that a contract needs to be measurable in terms of outcome and process. In addition, payers and industry stakeholders stated that a successful innovative contract must be controllable and that the payer and manufacturer must have established mutual interests.
From the stakeholder interviews and literature review, a summary of the key learnings can be summarised as follows:
Have an implementation methodology in place
It appears that many of the reasons for failure or dissatisfaction with innovative contracts are not necessarily due to the nature of innovative contracting itself, but more to the technical details of the implementation of contracts in the field. The challenges outlined above make it clear that having a solid methodology on exactly what type of innovative contract to implement in what scenario is critical, as is securing solid legal counsel to develop the contract.
Establish trust
It is vital that trust is established between all participants, after which defining a transparent mutual benefit is more straightforward. It was interesting in our research that payers are generally the more sceptical party about the benefits of innovative contracts when, in theory, such schemes should have the obvious benefit of reducing the payer’s budget. Therefore, it is essential that when developing an innovative contract, payers are involved from an early stage.
Simplify where possible
Greater simplicity in contract design and execution is beneficial. This may also help to ease the administrative burden that represents such an important barrier for the implementation of innovative contracting schemes. In addition, try to establish straightforward and easily measurable assessment criteria for the contract.
Involve physicians and patients
Most stakeholders suggested that physicians and patients should be more involved in the design of innovative contracts in the future. A better patient and physician understanding of the benefits of these schemes would ultimately provide more support and potentially better outcomes.
Establish a framework for success
Most importantly, we believe the development of a strategic framework that provides guidance for pharmaceutical companies in the design of innovative contracts is a critical success factor and can turn into a source of competitive advantage.
The research and analysis generated a set of critical insights, which in turn led to the design of a nuanced framework to identify the most suitable contracts that could be potentially implemented. The ideal design of an innovative contract can be defined through a blended analysis of therapeutic area, market and product profile characteristics; the so called ‘Innovative Contacting Excellence Framework’.
In summary, there is a clear need for innovative contracting. The current market conditions and growing importance of the payer absolutely dictate that. However currently, innovative contracts are too often designed and agreed upon without all the relevant factors being taken into consideration.
Companies can create a competitive edge when implementing innovative contracts. Expert guidance can help to establish a framework that fits with the company strategy, as well as establish access to payers to kick start successful implementation.





